IMS 2023: The Origins of Multiple Myeloma and Why it Matters
How does myeloma begin? This was one of the first topics discussed at the recent International Myeloma Society meeting held last week in Athens, Greece. Several speakers addressed this topic and why it is so important to answer this vital question.
Faith Davies, MD of NYU Langone, shared that learning more about the myeloma cell itself and the changes that happen in the immune system can lead to earlier treatment that might help patients avoid traditional myeloma therapy altogether.
Different Myeloma in Different Parts of the Body
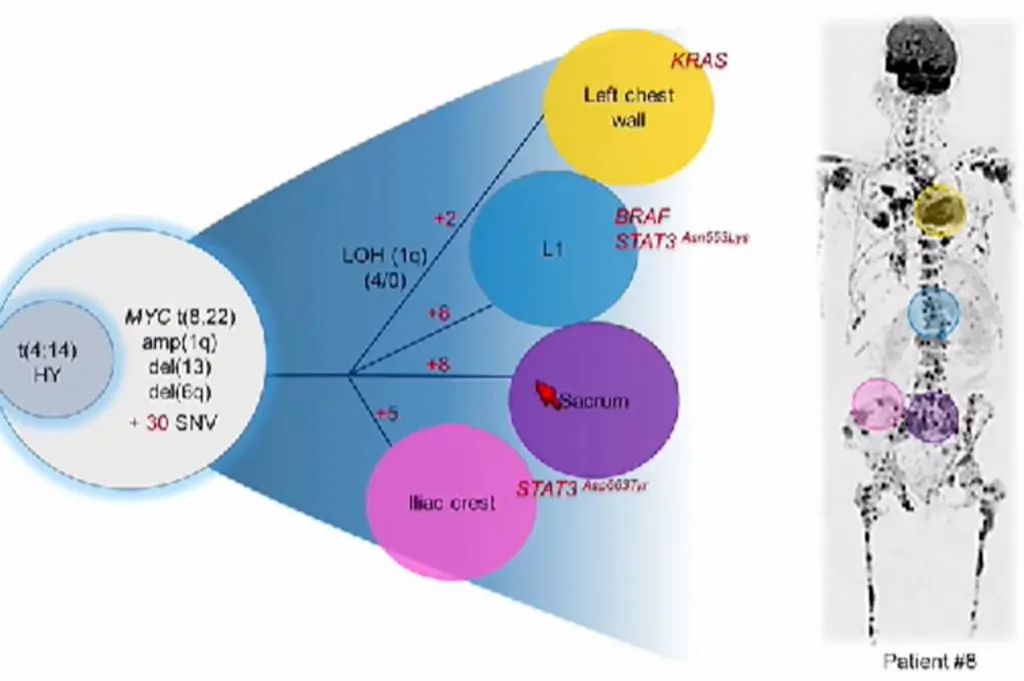
In her presentation, Dr. Davies showed how different genetic types of myeloma can be found in the body in different places. Even though some of the locations in the body share some genetic features, as the cells adapt to their new environment, each environment is different, creating different development of the myeloma over time in various parts of the body.
How Myeloma Begins and Evolves
- A genetic event happens. This can include gene translocations, where part of one gene swaps with another gene. Then copy number changes occur and other mutations occur.
- The first event happens in the second or third decade of a patient's life. Eight mutational signatures have been identified.
- Complex variants occur later in the process.
Leif Bergsagel, MD of Mayo Clinic, Scottsdale, shared that while normal myeloma cells are mature plasma cells, early undeveloped myeloma “stem cells” are the most likely cause of relapse. These stem cells were identified as early as 1968 by Dr. Bergsagel's father. Mature myeloma cells cannot replicate, while myeloma stem cells can. When patients are treated with myeloma therapy, the treatment kills the mature cells but not the stem cells.
Importantly the early stem cells already have mutations that Dr. Bergsagel believes were caused 20-40 years prior to a formal myeloma diagnosis. Myeloma is clearly a disease that has multiple trigger points in its development.
The Role of the Immune System That Allows Myeloma Growth
It's not just the myeloma cells but the status of a patient's immune system that creates further diversity and growth of the myeloma cells. Madhav Dhodapkar, MBBS of Emory University, provided a deep dive into the immune system and its role in myeloma cell growth. Using Gaucher's Disease as an example, he stated that if you can understand the driving factors, you can ultimately change or stop the course of the disease.
He stated that there were bacteria in the gut that acted as potential triggers for inflammation. These and other changes in the immune system originated early, even in an MGUS state with few cells. Those immune cells impacted the outcome and risk of myeloma development. The immune system reactions could be highly variable. Additional factors, like the "talking" between the cells and the bone marrow environment, also can impact the development.
He shared that while all MGUS precedes myeloma, it is not the first step in disease development. As MGUS develops into myeloma, the cells start to cluster together.
More knowledge about the underlying triggers as well as regaining immune system control, will be essential in preventing myeloma.
Why This Matters
If researchers can understand how the mutations occur, how the immune system fails to kill the early cancer cells, and how the disease evolves, earlier treatment could stop the disease before it grows to maturity. This is clearly essential work.
How does myeloma begin? This was one of the first topics discussed at the recent International Myeloma Society meeting held last week in Athens, Greece. Several speakers addressed this topic and why it is so important to answer this vital question.
Faith Davies, MD of NYU Langone, shared that learning more about the myeloma cell itself and the changes that happen in the immune system can lead to earlier treatment that might help patients avoid traditional myeloma therapy altogether.
Different Myeloma in Different Parts of the Body
In her presentation, Dr. Davies showed how different genetic types of myeloma can be found in the body in different places. Even though some of the locations in the body share some genetic features, as the cells adapt to their new environment, each environment is different, creating different development of the myeloma over time in various parts of the body.

How Myeloma Begins and Evolves
- A genetic event happens. This can include gene translocations, where part of one gene swaps with another gene. Then copy number changes occur and other mutations occur.
- The first event happens in the second or third decade of a patient's life. Eight mutational signatures have been identified.
- Complex variants occur later in the process.
Leif Bergsagel, MD of Mayo Clinic, Scottsdale, shared that while normal myeloma cells are mature plasma cells, early undeveloped myeloma “stem cells” are the most likely cause of relapse. These stem cells were identified as early as 1968 by Dr. Bergsagel's father. Mature myeloma cells cannot replicate, while myeloma stem cells can. When patients are treated with myeloma therapy, the treatment kills the mature cells but not the stem cells.
Importantly the early stem cells already have mutations that Dr. Bergsagel believes were caused 20-40 years prior to a formal myeloma diagnosis. Myeloma is clearly a disease that has multiple trigger points in its development.
The Role of the Immune System That Allows Myeloma Growth
It's not just the myeloma cells but the status of a patient's immune system that creates further diversity and growth of the myeloma cells. Madhav Dhodapkar, MBBS of Emory University, provided a deep dive into the immune system and its role in myeloma cell growth. Using Gaucher's Disease as an example, he stated that if you can understand the driving factors, you can ultimately change or stop the course of the disease.
He stated that there were bacteria in the gut that acted as potential triggers for inflammation. These and other changes in the immune system originated early, even in an MGUS state with few cells. Those immune cells impacted the outcome and risk of myeloma development. The immune system reactions could be highly variable. Additional factors, like the "talking" between the cells and the bone marrow environment, also can impact the development.
He shared that while all MGUS precedes myeloma, it is not the first step in disease development. As MGUS develops into myeloma, the cells start to cluster together.
More knowledge about the underlying triggers as well as regaining immune system control, will be essential in preventing myeloma.
Why This Matters
If researchers can understand how the mutations occur, how the immune system fails to kill the early cancer cells, and how the disease evolves, earlier treatment could stop the disease before it grows to maturity. This is clearly essential work.
about the author
Jennifer Ahlstrom
Myeloma survivor, patient advocate, wife, mom of 6. Believer that patients can contribute to cures by joining HealthTree Cure Hub and joining clinical research. Founder and CEO of HealthTree Foundation.
Trending Articles
Upcoming Events
Get the Latest Multiple Myeloma Updates, Delivered to You.
By subscribing to the HealthTree newsletter, you'll receive the latest research, treatment updates, and expert insights to help you navigate your health.
Together we care.
Together we cure.









