Tests for CLL Patients: Quantitative Immunoglobulins
One of the tests CLL patients can receive is called a quantitative immunoglobulins test. Immunoglobulins are antibodies, a protein that B-cells make to help fight infections. Antibodies help decrease infections by attaching to viruses, bacteria, and other pathogens present in the body’s blood and lymph fluid, limiting them from entering and infecting the body’s cells.
Image source: CellCartoons
The five types of antibodies (immunoglobulins) each have distinct functions and locations in the body. Each type of antibody has a unique structure and role, contributing to the body's ability to respond to a wide array of pathogens and other foreign substances.
- IgG (Immunoglobulin G)
- Function: IgG is the most abundant type of antibody in the body. It plays a crucial role in the body's immune response by neutralizing toxins and pathogens like viruses and bacteria. IgG antibodies are also essential in providing long-term immunity after an infection or vaccination
- Location: Found in all body fluids, IgG is particularly abundant in the blood and extracellular fluid
- Normal range: 700 to 1,500 mg/dL (milligrams per deciliter)
- IgA (Immunoglobulin A)
- Function: IgA primarily protects body surfaces that are exposed to outside substances. It is important in mucosal immunity, as it can prevent pathogens from adhering to and penetrating the mucous membranes
- Location: IgA is predominantly found in mucous membranes, such as those lining the respiratory and gastrointestinal tracts. It's also present in saliva, tears, and breast milk
- Normal range: 70 to 400 mg/dL
- IgM (Immunoglobulin M)
- Function: IgM is the first antibody type produced in response to an infection and is essential for primary immune response. It is effective in killing bacteria and activating complement system components, which enhances phagocytosis and inflammation
- Location: IgM is mainly found in the blood and lymph fluid
- Normal range: 40 to 230 mg/dL
- IgE (Immunoglobulin E)
- Function: IgE is associated with allergic reactions and is responsible for the immune response against parasites. It triggers histamine release from mast cells and basophils, leading to inflammation
- Location: IgE is found in the lungs, skin, and mucous membranes
- Normal range: 0.05 to 0.2 mg/dL
- IgD (Immunoglobulin D)
- Function: The exact role of IgD is not fully understood, but it is believed to play a role in the immune system's sensitization to antigens. It's also involved in the activation and regulation of B-cells
- Location: IgD is primarily found on the surface of B-cells and in small amounts in the blood
- Normal range: 0.3 to 40 mg/dL
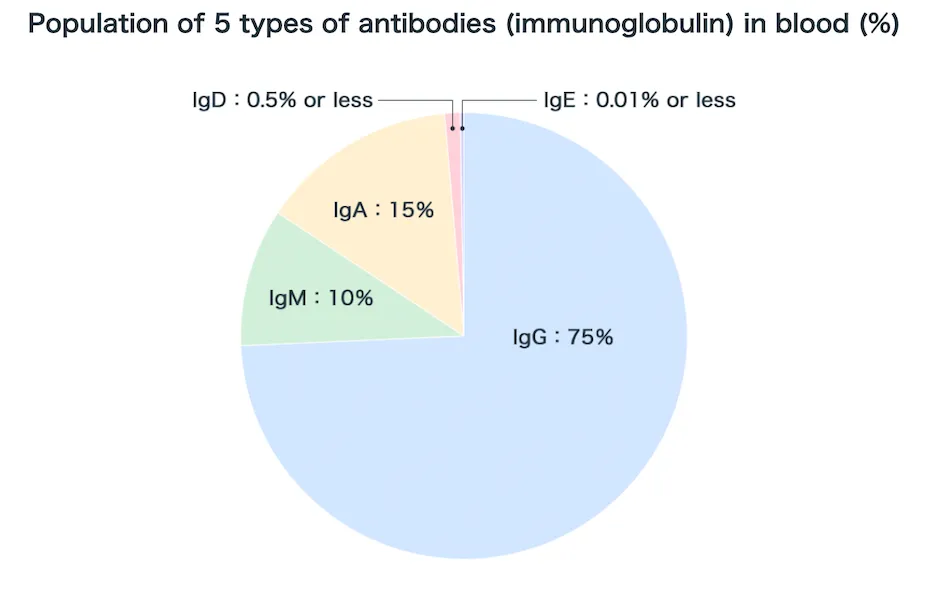
Image source: Kyowa Kirin
CLL patients may have decreased numbers of these antibodies due to the following reasons:
- Inherent disease mechanism: CLL primarily affects B-cells, which are responsible for producing antibodies. The cancerous B-cells in CLL are often dysfunctional and unable to produce normal levels of these antibodies
- Bone marrow suppression: CLL can crowd out normal bone marrow cells, including those that would otherwise become healthy B-cells. This suppression of normal marrow function can lead to reduced antibody production
- Treatment effects: Treatments for CLL may suppress the immune system. This suppression can affect the body's ability to produce antibodies, as these treatments may inadvertently target healthy B-cells along with the cancerous ones
- Secondary immune disorders: CLL patients are at an increased risk of developing other immune system disorders, which can further compromise their ability to produce normal levels of antibodies
- Advanced age: Many CLL patients are older, and the aging process naturally diminishes the immune system's efficacy, including the production of antibodies
- Infections: Chronic or repeated infections, which CLL patients are more susceptible to, can deplete the body's reserves of antibodies
It's important for CLL patients to be closely monitored for their antibody levels, as low levels can increase their risk for infections. Patients may be able to receive a donor antibody infusion called IVIG to help their immune system if their antibody levels are low. See here to learn more about IVIG for CLL patients.
Quantitative Immunoglobulins Test Steps
The procedure for a quantitative immunoglobulins test is straightforward and similar to a standard blood test. It involves these steps:
- Blood sample collection: A healthcare professional draws a small amount of blood from the patient's vein, typically from the arm
- Laboratory analysis: The collected blood is sent to a lab where the levels of different types of immunoglobulins (antibodies) are measured
- Result interpretation: The test results are analyzed to determine if the immunoglobulin levels are within a normal range, or if they are unusually high or low
Preparation for the Test
Generally, no special preparation is required for a quantitative immunoglobulins test. Patients can eat and drink normally and continue their medications unless instructed otherwise by their doctor. However, it's always advisable to follow any specific instructions provided by the healthcare provider.
Timeline for Test Results
The time taken to get results can vary depending on the laboratory's processing time. Typically, results are available within a few days to a week. Patients should consult with their healthcare provider for a more accurate timeline.
Analysis
It's important that the CLL patient consult with the healthcare professional who ordered the test to help interpret their test results. Their doctor can help take into account the patient’s overall health and CLL treatment history. Generally, low levels of antibodies indicate a weakened immune system, making patients more prone to infections. High levels of antibodies (uncommon) may indicate other conditions like chronic infections or other types of immune system disorders.
Conclusion
The quantitative immunoglobulins test is a helpful tool that can provide insight into the patient’s immune system health, helping doctors make informed decisions about treatment and preventive care. CLL patients should reach out to their doctor regarding any questions they have related to the test or interpreting its results.
One of the tests CLL patients can receive is called a quantitative immunoglobulins test. Immunoglobulins are antibodies, a protein that B-cells make to help fight infections. Antibodies help decrease infections by attaching to viruses, bacteria, and other pathogens present in the body’s blood and lymph fluid, limiting them from entering and infecting the body’s cells.

Image source: CellCartoons
The five types of antibodies (immunoglobulins) each have distinct functions and locations in the body. Each type of antibody has a unique structure and role, contributing to the body's ability to respond to a wide array of pathogens and other foreign substances.
- IgG (Immunoglobulin G)
- Function: IgG is the most abundant type of antibody in the body. It plays a crucial role in the body's immune response by neutralizing toxins and pathogens like viruses and bacteria. IgG antibodies are also essential in providing long-term immunity after an infection or vaccination
- Location: Found in all body fluids, IgG is particularly abundant in the blood and extracellular fluid
- Normal range: 700 to 1,500 mg/dL (milligrams per deciliter)
- IgA (Immunoglobulin A)
- Function: IgA primarily protects body surfaces that are exposed to outside substances. It is important in mucosal immunity, as it can prevent pathogens from adhering to and penetrating the mucous membranes
- Location: IgA is predominantly found in mucous membranes, such as those lining the respiratory and gastrointestinal tracts. It's also present in saliva, tears, and breast milk
- Normal range: 70 to 400 mg/dL
- IgM (Immunoglobulin M)
- Function: IgM is the first antibody type produced in response to an infection and is essential for primary immune response. It is effective in killing bacteria and activating complement system components, which enhances phagocytosis and inflammation
- Location: IgM is mainly found in the blood and lymph fluid
- Normal range: 40 to 230 mg/dL
- IgE (Immunoglobulin E)
- Function: IgE is associated with allergic reactions and is responsible for the immune response against parasites. It triggers histamine release from mast cells and basophils, leading to inflammation
- Location: IgE is found in the lungs, skin, and mucous membranes
- Normal range: 0.05 to 0.2 mg/dL
- IgD (Immunoglobulin D)
- Function: The exact role of IgD is not fully understood, but it is believed to play a role in the immune system's sensitization to antigens. It's also involved in the activation and regulation of B-cells
- Location: IgD is primarily found on the surface of B-cells and in small amounts in the blood
- Normal range: 0.3 to 40 mg/dL

Image source: Kyowa Kirin
CLL patients may have decreased numbers of these antibodies due to the following reasons:
- Inherent disease mechanism: CLL primarily affects B-cells, which are responsible for producing antibodies. The cancerous B-cells in CLL are often dysfunctional and unable to produce normal levels of these antibodies
- Bone marrow suppression: CLL can crowd out normal bone marrow cells, including those that would otherwise become healthy B-cells. This suppression of normal marrow function can lead to reduced antibody production
- Treatment effects: Treatments for CLL may suppress the immune system. This suppression can affect the body's ability to produce antibodies, as these treatments may inadvertently target healthy B-cells along with the cancerous ones
- Secondary immune disorders: CLL patients are at an increased risk of developing other immune system disorders, which can further compromise their ability to produce normal levels of antibodies
- Advanced age: Many CLL patients are older, and the aging process naturally diminishes the immune system's efficacy, including the production of antibodies
- Infections: Chronic or repeated infections, which CLL patients are more susceptible to, can deplete the body's reserves of antibodies
It's important for CLL patients to be closely monitored for their antibody levels, as low levels can increase their risk for infections. Patients may be able to receive a donor antibody infusion called IVIG to help their immune system if their antibody levels are low. See here to learn more about IVIG for CLL patients.
Quantitative Immunoglobulins Test Steps
The procedure for a quantitative immunoglobulins test is straightforward and similar to a standard blood test. It involves these steps:
- Blood sample collection: A healthcare professional draws a small amount of blood from the patient's vein, typically from the arm
- Laboratory analysis: The collected blood is sent to a lab where the levels of different types of immunoglobulins (antibodies) are measured
- Result interpretation: The test results are analyzed to determine if the immunoglobulin levels are within a normal range, or if they are unusually high or low
Preparation for the Test
Generally, no special preparation is required for a quantitative immunoglobulins test. Patients can eat and drink normally and continue their medications unless instructed otherwise by their doctor. However, it's always advisable to follow any specific instructions provided by the healthcare provider.
Timeline for Test Results
The time taken to get results can vary depending on the laboratory's processing time. Typically, results are available within a few days to a week. Patients should consult with their healthcare provider for a more accurate timeline.
Analysis
It's important that the CLL patient consult with the healthcare professional who ordered the test to help interpret their test results. Their doctor can help take into account the patient’s overall health and CLL treatment history. Generally, low levels of antibodies indicate a weakened immune system, making patients more prone to infections. High levels of antibodies (uncommon) may indicate other conditions like chronic infections or other types of immune system disorders.
Conclusion
The quantitative immunoglobulins test is a helpful tool that can provide insight into the patient’s immune system health, helping doctors make informed decisions about treatment and preventive care. CLL patients should reach out to their doctor regarding any questions they have related to the test or interpreting its results.

about the author
Megan Heaps
Megan joined HealthTree in 2022. She enjoys helping patients and their care partners understand the various aspects of the cancer. This understanding enables them to better advocate for themselves and improve their treatment outcomes.
More on Navigating Your Health
Get the Latest Chronic Lymphocytic Leukemia Updates, Delivered to You.
By subscribing to the HealthTree newsletter, you'll receive the latest research, treatment updates, and expert insights to help you navigate your health.
Together we care.
Together we cure.