Better Sleep With Cancer: Understanding Sleep Problems and How to Rest Better

Sleep plays a vital role in physical health, emotional balance, and recovery. It is a biological necessity for people to function properly. For people with cancer, sleep is an important part of overall health. On this page, you’ll learn how sleep can help you recover, how sleep disorders affect people with cancer and their caregivers, and how to improve sleep hygiene and sleep quality.
What is the importance of sleep?
Sleep is a fundamental biological process. It regulates immune function, hormonal balance, and cellular repair. During sleep, particularly deep sleep, the body increases production of immune signaling molecules called cytokines. These help coordinate immune defense. Sleep also helps regulate inflammation, which is critical in preventing chronic disease and maintaining overall health.
In people with cancer, sleep problems are very common. Even though people with cancer are more likely to have sleep problems than the general population, they are often under-recognized in cancer care. But sleep has a large impact on your health. It influences how well your immune system works and affects your quality of life. Prioritizing healthy sleep patterns and getting help for your sleep problems is an essential part of maintaining your during and after cancer treatment.
What is the sleep cycle?
The sleep cycle is made up of the different stages that happen after you fall asleep. They happen in 90 to 110 minute stages throughout the night. In the earlier stages, you get deeper sleep, which supports physical restoration. Later, you get more REM sleep, which contributes to mental and emotional restoration.
In the first half of your sleep cycle, the body spends more time in deep non–rapid eye movement (NREM) sleep. This stage is essential for physical restoration. During NREM sleep:
- Heart rate and blood pressure decrease
- Muscles fully relax
- Growth hormone is released
- The immune system becomes more active.
NREM sleep is when tissue repair, muscle recovery, cellular healing, and energy replenishment primarily occur.
- Early night = more deep sleep (physical restoration)
- Late night = more REM sleep (mental and emotional restoration)
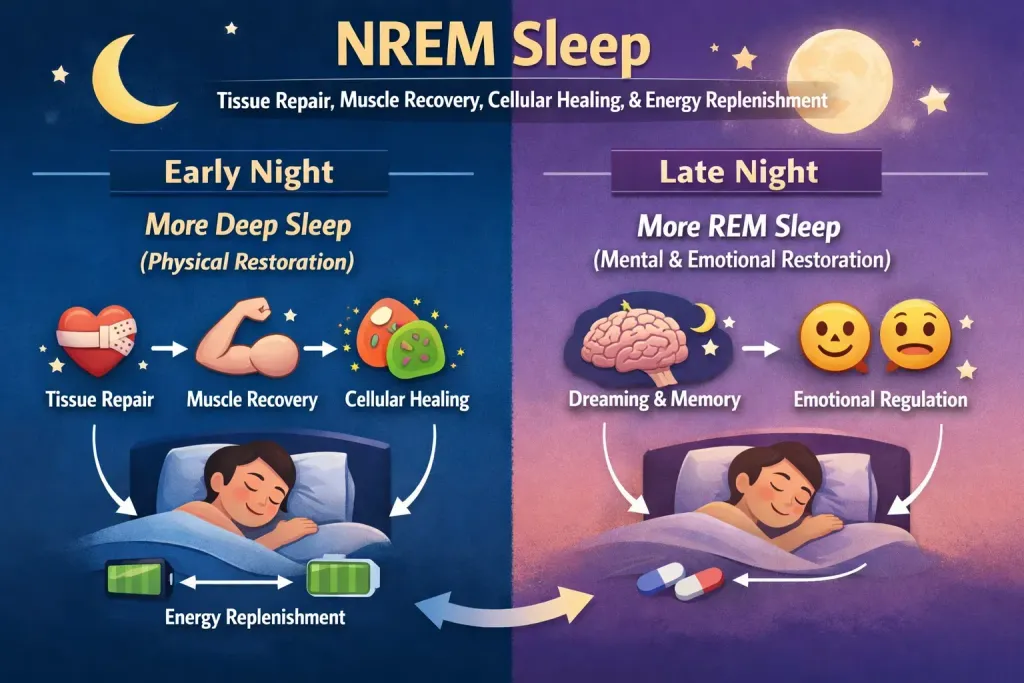
In the second half of your sleep cycle, rapid eye movement (REM) sleep becomes longer and more frequent. REM sleep is critical for brain restoration. It supports memory consolidation, emotional processing, learning, and mood regulation. While deep sleep restores the body, REM sleep restores the mind.
One full cycle lasts about 90 to 110 minutes. Completing 4 to 6 full sleep cycles per night allows both physical and mental recovery systems to function properly. For the best sleep, you need both deep sleep and REM sleep. This is why getting a full 7 to 9 hours of uninterrupted sleep is important.
Sleep Phases Include:
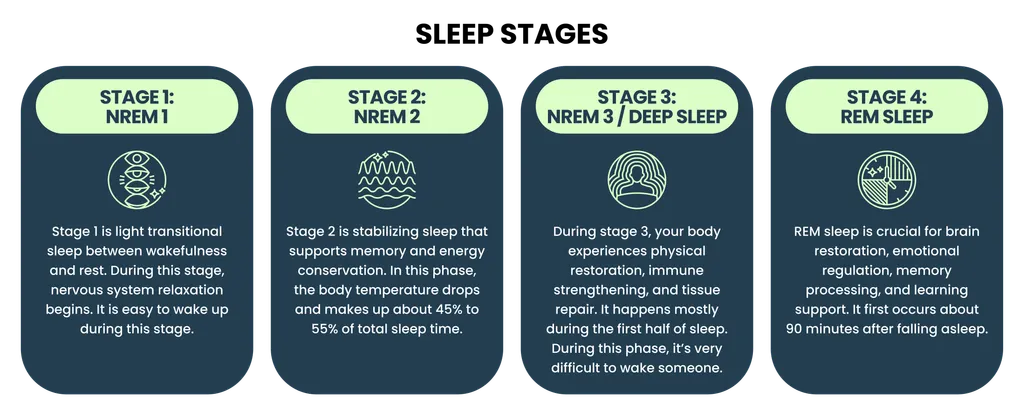
- Stage 1 (NREM 1): Stage 1 is light transitional sleep between wakefulness and rest. During this stage, nervous system relaxation begins. It is easy to wake up during this stage.
- Stage 2 (NREM 2): Stage 2 is stabilizing sleep that supports memory and energy conservation. In this phase, the body temperature drops and makes up about 45% to 55% of total sleep time.
- Stage 3 (NREM 3 / Deep Sleep): During stage 3, your body experiences physical restoration, immune strengthening, and tissue repair. It happens mostly during the first half of sleep. During this phase, it’s very difficult to wake someone.
- REM Sleep: REM sleep is crucial for brain restoration, emotional regulation, memory processing, and learning support. It first occurs about 90 minutes after falling asleep.
How sleep supports physical and emotional recovery
Physically, sleep helps the body heal. Sleep promotes:
- Tissue repair
- Immune surveillance
- Hormonal regulation
During sleep, immune cells become more active. This helps the body detect and eliminate abnormal or damaged cells. Sleep also reduces sympathetic nervous system activity and lowers stress hormones like cortisol. This creates conditions that support healing and recovery.
Sleep can also help stabilize your mood and help you think better. For people with cancer, sleep problems are associated with depression, anxiety, and reduced quality of life.
Emotional distress and sleep problems can reinforce each other. Improving sleep may also help you cope and improve your overall well-being during diagnosis and treatment.
The body’s internal clock is called the circadian rhythm
The circadian rhythm is the body’s internal 24-hour timing system. It regulates sleep-wake cycles, hormone secretion, and immune activity. Brain structures that respond to light and darkness coordinate your circadian rhythm and regulate melatonin production. Melatonin is a hormone. It not only signals the body to prepare for sleep but also plays a role in the immune system.

When your natural circadian rhythm is disrupted, it can affect your immune system and cellular functions. During circadian rhythm sleep disorders, the body’s internal clock is misaligned with the external day–night cycle. This can happen due to:
- Irregular sleep schedules
- Shift work
- Frequent hospitalizations
- Reduced exposure to natural light
When your circadian rhythm is disrupted, your hormone cycles and sleep timing are disrupted, too. This can make it difficult to fall asleep at normal times, causing you to wake up too early or to wake up often throughout the night. Over time, circadian disruption can affect your mood, how well your immune system works, and your overall health.
Improving your sleep hygiene can help. Sleep hygiene refers to your sleep habits. You can limit light exposure at night, avoid using screens close to bedtime, and gradually adjust your sleep and wake times. Timed light exposure, like bright light therapy, in the morning can help. Melatonin supplements may be used at carefully timed intervals to help shift circadian rhythms.
Why disrupted sleep can worsen fatigue, pain, and mood
Sleep problems are often part of a symptom cluster in cancer that includes:
- Fatigue
- Pain
- Depression
When sleep is interrupted or shortened, you are less alert during the day. You may feel more distracted and experience fatigue. This can create a cycle that makes it difficult to get good sleep. Your low energy reduces activity levels, which makes it more difficult to sleep well at night.
Poor sleep can also make inflammation worse. This can make you more sensitive to pain and worsen mood symptoms. A study of people with cancer-related fatigue found that a good sleep schedule improved symptoms.
Why do people with cancer have sleep problems?
Sleep problems happen for many different reasons across all phases of cancer care, including before treatment begins, during active therapy, and into survivorship.
Sleep problems in cancer patients often develop from a combination of physical symptoms, emotional stress, biological changes, and environmental changes. These factors can also overlap.
The most common causes of sleep disorders for people with cancer include:
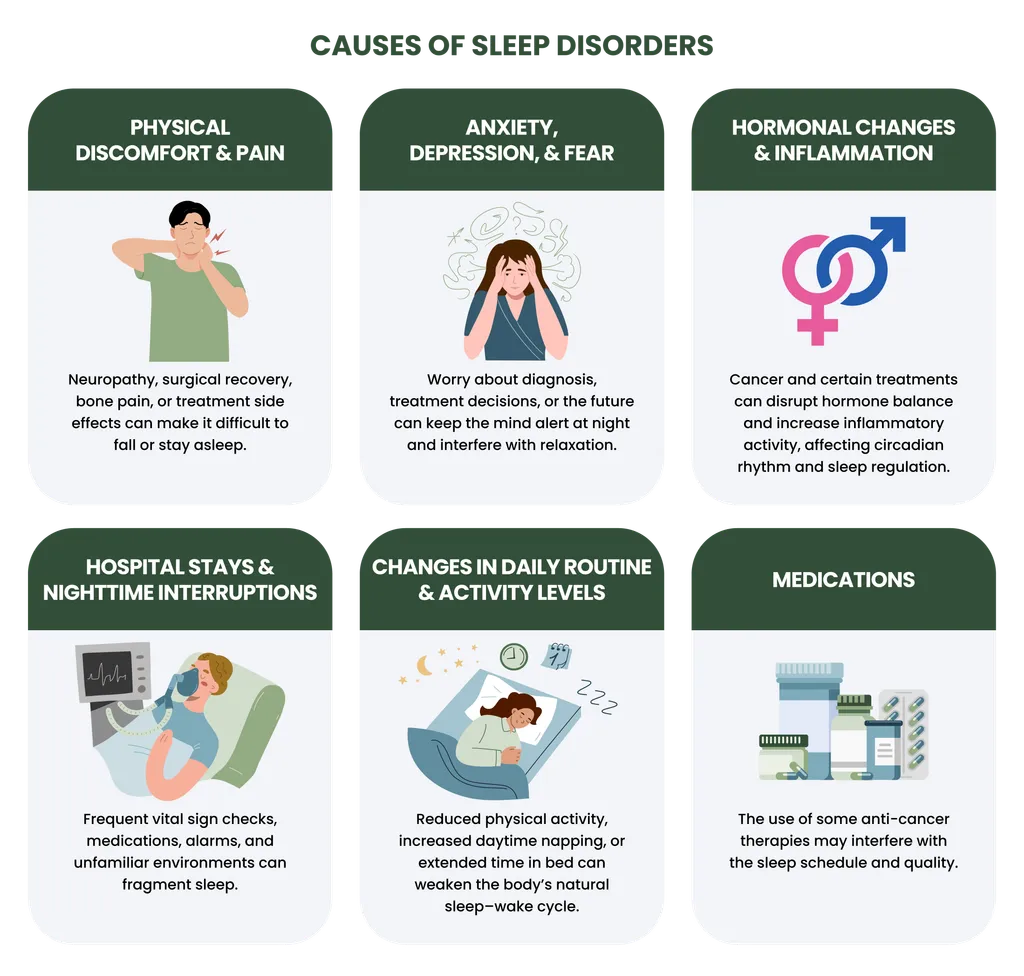
- Physical discomfort and pain. Neuropathy, surgical recovery, bone pain, or treatment side effects can make it difficult to fall or stay asleep.
- Anxiety, depression, and fear. Worry about diagnosis, treatment decisions, or the future can keep the mind alert at night and interfere with relaxation.
- Hormonal changes and inflammation. Cancer and certain treatments can disrupt hormone balance and increase inflammatory activity, affecting circadian rhythm and sleep regulation.
- Hospital stays and nighttime interruptions. Frequent vital sign checks, medications, alarms, and unfamiliar environments can fragment sleep.
- Changes in daily routine and activity levels. Reduced physical activity, increased daytime napping, or extended time in bed can weaken the body’s natural sleep–wake cycle.
- Medications. The use of some anti-cancer therapies may interfere with the sleep schedule and quality.
How do cancer treatments affect sleep?
Cancer treatments can affect sleep in different ways depending on how they interact with the body, immune system, hormones, and nervous system.
Some treatments directly disrupt sleep cycles. Others worsen symptoms like pain, fatigue, or inflammation that interfere with rest. Understanding these effects can help you anticipate changes and work with your care team to protect your sleep quality during treatment.
Chemotherapy
Chemotherapy causes many different side effects, such as nausea, pain, neuropathy, night sweats, or gastrointestinal upset, that can make it hard to stay asleep. Chemotherapy can also increase inflammation and alter circadian rhythms, leading to fragmented sleep or insomnia. It can also cause anxiety surrounding treatment cycles that further disrupt nighttime rest.
Radiation therapy
Radiation therapy is commonly associated with significant fatigue. But this fatigue does not always make it easy to get restful sleep. You may feel exhausted during the day but struggle with nighttime insomnia.
Radiation can also irritate nearby tissues, causing discomfort or inflammation that makes it hard to fall asleep or stay asleep. Over time, disrupted sleep may intensify the cycle of daytime fatigue and nighttime wakefulness.
Immunotherapy
Immunotherapy works by stimulating the immune system to recognize and attack cancer cells. However, this immune activation can increase inflammatory signaling in the body.
Elevated inflammation has been linked to changes in sleep patterns. It can cause increased nighttime awakenings and excessive daytime sleepiness. Flu-like side effects such as fever, chills, or body aches may also temporarily disrupt sleep.
Surgery
Surgery can significantly alter sleep patterns, especially in the immediate recovery period. Pain, limited mobility, hospital monitoring, and anesthesia effects can interrupt sleep. Inflammation and stress responses after surgery may also disrupt circadian rhythms. Some patients have temporary changes in sleep depth and REM sleep as the body recovers from surgical stress.
Steroids and stimulant effects on sleep
Corticosteroids like dexamethasone are commonly used to reduce inflammation, prevent nausea, or manage treatment side effects. These medications can also strongly affect sleep. The body produces a corticosteroid hormone during sleep called cortisol.
When a corticosteroid is used, it may increase alertness, elevate heart rate, and raise energy levels, particularly when taken later in the day. As a result, patients may have difficulty falling asleep, frequent awakenings, or a feeling of being “wired but tired.” If any of these side effects happen to you after taking one of these treatments, talk to your doctor and see if adjusting timing or dosing can help reduce these effects.
Sleep changes during treatment are common and do not mean something is “wrong.” Recognizing these patterns early allows patients and providers to take proactive steps to protect rest, energy, and overall well-being.
What are the different types of sleep disorders?
Sleep disorders are medical conditions that disrupt the ability to fall asleep, stay asleep, or obtain restorative sleep. They can affect any part of the sleep cycle, including the duration and schedule of your sleep, how well you breathe during sleep, how much you move during sleep, and your overall sleep quality.
These problems can lead to fatigue, mood changes, thinking and memory problems, and reduced physical functioning.
Insomnia
Insomnia is the most common sleep disorder. It involves ongoing problems:
- Falling asleep
- Staying asleep
- Waking too early
- Being unable to fall back asleep
Insomnia can be short-term or long-term. Long-term insomnia lasts three months or longer.
Insomnia often leads to fatigue, irritability, difficulty concentrating, and emotional distress. In people undergoing cancer treatment, insomnia may be triggered by anxiety, pain, hospital routines, corticosteroids, or changes in daily schedule.
The first-line treatment for chronic insomnia is cognitive behavioral therapy for insomnia (CBT-I). This is a type of therapy that focuses on understanding thoughts and behaviors around sleep.
Short-term use of sleep medications may be considered during acute stress or medical treatment, but behavioral therapy remains the most effective long-term strategy.
Sleep apnea
Sleep apnea is a breathing-related sleep disorder. During sleep apnea, airflow repeatedly stops and starts during sleep. The most common type is obstructive sleep apnea. It happens when throat muscles relax and block the airway. These pauses in breathing reduce oxygen levels and briefly wake the brain multiple times per hour, even if the person does not remember waking.
Symptoms include:
- Loud snoring.
- Gasping during sleep.
- Morning headaches.
- Excessive daytime sleepiness.
Untreated sleep apnea can increase the risk of cardiovascular problems and worsen fatigue. A treatment for sleep apnea is addressing airway obstruction and improving nighttime breathing.
The most common and effective treatment is continuous positive airway pressure (CPAP), a device that keeps the airway open by delivering steady air pressure through a mask.

Other options include oral appliances fitted by dental specialists, weight management, and positional therapy. In some cases, surgery may be recommended. Treating sleep apnea often improves daytime energy, cardiovascular health, and cognitive function.
Restless legs syndrome (RLS)
Restless legs syndrome is a neurological condition. It is characterized by an uncomfortable urge to move the legs, usually in the evening or at night. People often describe sensations such as tingling, crawling, or pulling that improve with movement. Because symptoms worsen during rest, RLS can make it harder to fall asleep and cause you to wake up frequently. Iron deficiency, nerve damage, or certain medications can contribute to symptoms.
Treatment for RLS focuses on relieving uncomfortable sensations so you can stay asleep. Ways to treat RLS include:
- Fixing iron deficiency when present.
- Reducing caffeine and alcohol intake
- Maintaining regular sleep schedules.
- Moderate exercise and leg stretching may also help.
In moderate to severe cases, medications such as dopamine agonists, gabapentin, or other nerve-calming agents may be prescribed to reduce symptoms.
Excessive daytime sleepiness and cancer-related fatigue
Excessive daytime sleepiness refers to persistent drowsiness and an inability to stay awake during normal waking hours, often caused by poor-quality nighttime sleep or underlying sleep disorders.
Cancer-related fatigue, while sometimes overlapping, is a distinct and often more intense exhaustion. It is not fully relieved by rest. It may be driven by inflammation, anemia, treatment side effects, emotional stress, and disrupted sleep.
Treatment depends on what is causing your sleep problems. If excessive sleepiness is due to sleep apnea, insomnia, or medication side effects, addressing those conditions can significantly improve alertness. Cancer-related fatigue may require a multifaceted approach, including:
- Managing anemia
- Controlling pain
- Engaging in light physical activity
- Improving nighttime sleep quality
- Addressing emotional distress.
- Energy conservation strategies
- Structured daytime activity
How are sleep disorders diagnosed?
Sleep disorders are diagnosed through a combination of health history, symptom questionnaires, sleep diaries, and sometimes specialized testing. A diagnosis can help find the best therapy to improve your quality of life.
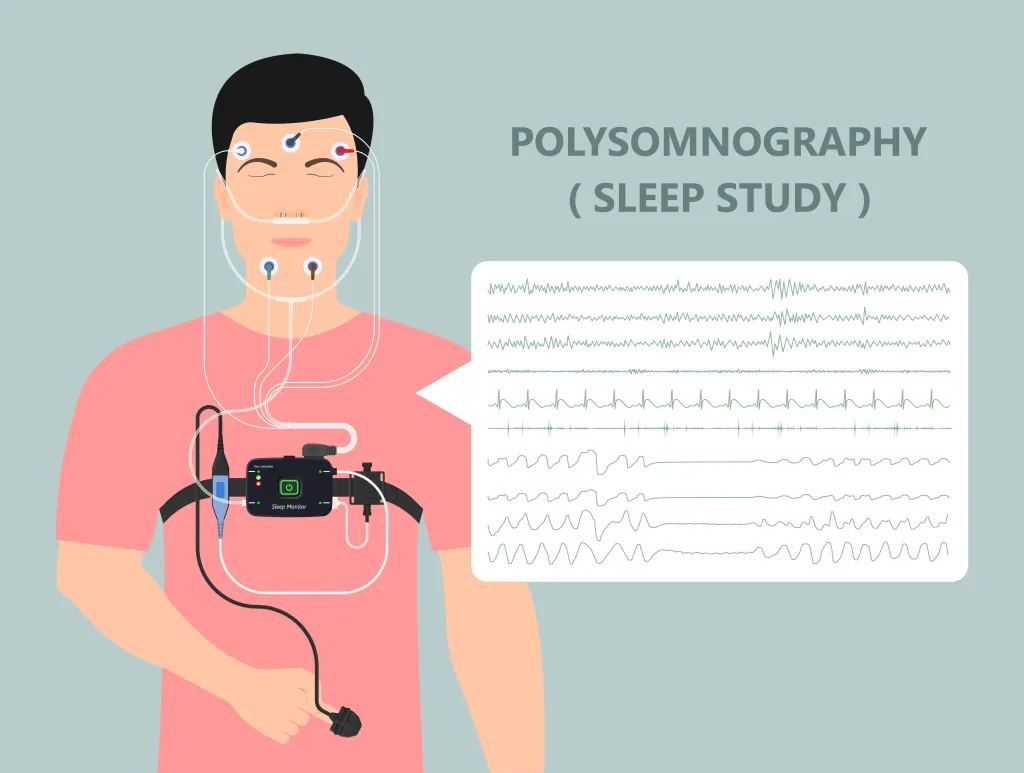
A healthcare provider will ask about sleep patterns, daytime symptoms, medical history, and medications. You may be asked to track sleep habits for several weeks. You may have a specialized test called the polysomnography. This is an overnight sleep study that helps identify sleep cycles and breathing patterns during sleep. Another option if sleep apnea is suspected is a home sleep apnea test. This can be done to monitor breathing, oxygen levels, heart rate, and brain activity during sleep.
What are natural ways to improve sleep quality?
There are medications that can help you sleep, but they do have some risks. These include a risk of dependency and thinking and memory (cognitive) problems. Before using sleep medications, your healthcare team will help you try other approaches. Changing your habits is often the most effective long-term solution for treating sleep disorders, especially insomnia.
Non-medical therapies focus on retraining the brain and body to associate the bed with sleep, regulating the circadian rhythm, and reducing physical and emotional stimuli at night. Unlike medications, behavioral strategies address the root causes of your sleep problems. They can provide lasting improvement. Below are evidence-based approaches without medication that can significantly improve sleep quality.
Cognitive behavioral therapy for insomnia (CBT-I)
CBT-I is considered the gold standard treatment for chronic insomnia. It helps identify and change thoughts and behaviors that interfere with sleep. CBT-I often includes:
- Stimulus control. This technique helps people with insomnia change negative associations they may have with the bed and the bedroom.
- Sleep restriction therapy. This is changing sleep so it happens in a consistent window. Cognitive restructuring. This is identifying and challenging negative beliefs and anxious thoughts about sleep.
- Relaxation training.
CBT-I is highly effective and produces durable results without medication side effects.This therapy needs professional counseling and commitment to slowly make permanent changes in habits with the purpose of getting used to these new habits and sleeping better.
Relaxation techniques and mindfulness
Stress is one of the main causes of insomnia. Relaxation practices such as progressive muscle relaxation, guided imagery, body scans, and mindfulness meditation help calm the nervous system before bedtime. These techniques reduce cortisol levels, slow heart rate, and create the mental shift necessary for sleep onset.
Methods such as diaphragmatic breathing or slow breathing techniques can lower heart rate and reduce anxiety at bedtime. Breathing exercises are simple, portable tools that can be used during nighttime awakenings as well.
Physical activity can help regulate your sleep schedule
Light physical activity during the day helps you fall asleep and improves overall sleep quality. Gentle evening stretching, restorative yoga, or slow mobility exercises can help release muscle tension and reduce discomfort. Regular daytime exercise can support deeper sleep, though vigorous workouts close to bedtime may be stimulating for some people.
Regulating the circadian rhythm with light
Light is the most powerful regulator of the body’s internal clock. Morning exposure to natural sunlight helps signal wakefulness and strengthens circadian alignment. In contrast, limiting bright light and screen exposure in the evening supports melatonin production. For people with circadian rhythm disruptions, structured light exposure and consistent wake times are especially important for stabilizing sleep patterns.
For example, new devices such as sunrise alarms can help regulate the circadian cycle with only light therapy.
What is sleep hygiene? How a good nighttime sleep routine can be life-changing
Sleep hygiene refers to daily habits and environmental practices that promote restorative sleep. While sleep hygiene alone may not cure chronic insomnia, it forms the foundation for healthy sleep. Over time, consistency strengthens the brain’s association between bed and rest.
The tips below can help you improve your sleep hygiene and get better, more restful sleep.
Create a cozy environment in your bedroom
- Keep the bedroom cool, dark, and quiet to help your body wind down.
- Choose a comfortable mattress, pillows, and bedding that support restful sleep.
- Reserve your bed for sleep only, not work or TV, so your brain associates it with rest.
Adhere to a consistent bedtime
- Go to sleep and wake up at the same times every day, even weekends.
- Avoid long or late naps that can make it harder to fall asleep at night.
Prepare your body for sleeping
- Wind down with relaxing activities before bed, such as reading, gentle stretching, or listening to soothing music.
- Disconnect from screens such as phones, tablets, computers, and TVs at least 30 to 60 minutes before bed. This is because blue light from screens can delay melatonin production and keep you awake.
- If you can’t fall asleep after around 20 minutes in bed, get up and do something calming in dim light until you feel sleepy again.
Small daily habits make a big difference
- Get daylight exposure to help regulate your sleep–wake rhythm.
- Keep active with regular exercise (but avoid intense workouts too close to bedtime).
- Avoid caffeine and alcohol in the hours before sleep, and avoid heavy meals close to bedtime.
Is napping helpful or harmful?
Napping can be helpful if done at the right time and for the right duration. Short naps between 20 and 30 minutes earlier in the day may improve alertness without interfering with nighttime sleep. For those experiencing cancer-related fatigue, carefully timed brief naps may support energy while preserving nighttime rest.
However, napping for too long or too late during the day can further affect sleep disorders, making it harder to fall asleep at night. For people struggling with insomnia, limiting or eliminating daytime naps is often recommended.
When should you talk to your healthcare team about sleep?
Sleep problems are common during and after cancer treatment, but persistent or severe disturbances should not be ignored. Research shows that sleep disruption can worsen fatigue, mood changes, pain perception, and overall quality of life , and may also be linked to immune and inflammatory changes. Because sleep plays a role in recovery and treatment tolerance, discussing concerns early allows for proper evaluation and targeted support.
You should always talk to your healthcare team about sleep problems, even if they seem minor.
There are some signs that your sleep problems might be more serious. Talk to your health care team right away if you experience:
- Difficulty falling or staying asleep three or more nights per week
- Loud snoring, gasping, or pauses in breathing during sleep
- Persistent daytime sleepiness that interferes with daily functioning
- Severe fatigue that does not improve with rest
- Restless, uncomfortable sensations in the legs at night
- Mood changes (increased anxiety, irritability, or depression) linked to poor sleep
- Sleep disruption that continues for weeks or worsens during treatment
These signs may indicate insomnia, sleep apnea, restless legs syndrome, circadian rhythm disruption, or treatment-related sleep changes that require medical attention.
What to ask your care team
Open communication can lead to better and faster solutions. Clearing your questions with your healthcare team can help them analyze what may be interfering with your rest.
- Could my treatment or medications be affecting my sleep?
- Should I be evaluated for a sleep disorder?
- Would cognitive behavioral therapy for insomnia (CBT-I) help me?
- Are there safe sleep aids or alternatives I can use?
- Could my fatigue be related to a sleep problem rather than just treatment?
Keep in mind that before self-medicating with sleep medications, there are many changes that don’t require medication and are proven effective against sleep disorders. Always ask your team before considering a new medication, and keep open communication with your loved ones to provide better support with daily routines around bedtime.
Sleep is a biologically essential process. It supports immune regulation, tissue repair, emotional balance, cognitive function, and overall resilience. Throughout this article, we’ve explored how sleep cycles restore the body and brain, how cancer and its treatments can disrupt normal sleep patterns, and how untreated sleep problems can worsen fatigue, pain, mood changes, and quality of life.
If you are struggling with sleep, don’t wait. Bring it up at your next appointment. Sleep problems are common during cancer care, and they are treatable. Ask your healthcare team about screening for sleep disorders, behavioral therapies like CBT-I, or strategies to improve your sleep routine.
Visit HealthTree’s Side Effect Solutions to see what has worked for others or create an account to contribute with what has worked for you!
CREATE YOUR HEALTHTREE ACCOUNT
Sources:
- Good Sleep for Good Health
- Sleep duration and the risk of cancer: a systematic review and meta-analysis including dose–response relationship
- The Triad of Sleep, Immunity, and Cancer: A Mediating Perspective
- Sleep disorders and cancer: State of the art and future perspectives
- Sleep/Wake Disturbances in People With Cancer and Their Caregivers: State of the Science
- Physiology, Sleep Stages
- Why Is Sleep Important?
Sleep plays a vital role in physical health, emotional balance, and recovery. It is a biological necessity for people to function properly. For people with cancer, sleep is an important part of overall health. On this page, you’ll learn how sleep can help you recover, how sleep disorders affect people with cancer and their caregivers, and how to improve sleep hygiene and sleep quality.
What is the importance of sleep?
Sleep is a fundamental biological process. It regulates immune function, hormonal balance, and cellular repair. During sleep, particularly deep sleep, the body increases production of immune signaling molecules called cytokines. These help coordinate immune defense. Sleep also helps regulate inflammation, which is critical in preventing chronic disease and maintaining overall health.
In people with cancer, sleep problems are very common. Even though people with cancer are more likely to have sleep problems than the general population, they are often under-recognized in cancer care. But sleep has a large impact on your health. It influences how well your immune system works and affects your quality of life. Prioritizing healthy sleep patterns and getting help for your sleep problems is an essential part of maintaining your during and after cancer treatment.
What is the sleep cycle?
The sleep cycle is made up of the different stages that happen after you fall asleep. They happen in 90 to 110 minute stages throughout the night. In the earlier stages, you get deeper sleep, which supports physical restoration. Later, you get more REM sleep, which contributes to mental and emotional restoration.
In the first half of your sleep cycle, the body spends more time in deep non–rapid eye movement (NREM) sleep. This stage is essential for physical restoration. During NREM sleep:
- Heart rate and blood pressure decrease
- Muscles fully relax
- Growth hormone is released
- The immune system becomes more active.
NREM sleep is when tissue repair, muscle recovery, cellular healing, and energy replenishment primarily occur.
- Early night = more deep sleep (physical restoration)
- Late night = more REM sleep (mental and emotional restoration)

In the second half of your sleep cycle, rapid eye movement (REM) sleep becomes longer and more frequent. REM sleep is critical for brain restoration. It supports memory consolidation, emotional processing, learning, and mood regulation. While deep sleep restores the body, REM sleep restores the mind.
One full cycle lasts about 90 to 110 minutes. Completing 4 to 6 full sleep cycles per night allows both physical and mental recovery systems to function properly. For the best sleep, you need both deep sleep and REM sleep. This is why getting a full 7 to 9 hours of uninterrupted sleep is important.
Sleep Phases Include:
- Stage 1 (NREM 1): Stage 1 is light transitional sleep between wakefulness and rest. During this stage, nervous system relaxation begins. It is easy to wake up during this stage.
- Stage 2 (NREM 2): Stage 2 is stabilizing sleep that supports memory and energy conservation. In this phase, the body temperature drops and makes up about 45% to 55% of total sleep time.
- Stage 3 (NREM 3 / Deep Sleep): During stage 3, your body experiences physical restoration, immune strengthening, and tissue repair. It happens mostly during the first half of sleep. During this phase, it’s very difficult to wake someone.
- REM Sleep: REM sleep is crucial for brain restoration, emotional regulation, memory processing, and learning support. It first occurs about 90 minutes after falling asleep.

How sleep supports physical and emotional recovery
Physically, sleep helps the body heal. Sleep promotes:
- Tissue repair
- Immune surveillance
- Hormonal regulation
During sleep, immune cells become more active. This helps the body detect and eliminate abnormal or damaged cells. Sleep also reduces sympathetic nervous system activity and lowers stress hormones like cortisol. This creates conditions that support healing and recovery.
Sleep can also help stabilize your mood and help you think better. For people with cancer, sleep problems are associated with depression, anxiety, and reduced quality of life.
Emotional distress and sleep problems can reinforce each other. Improving sleep may also help you cope and improve your overall well-being during diagnosis and treatment.
The body’s internal clock is called the circadian rhythm
The circadian rhythm is the body’s internal 24-hour timing system. It regulates sleep-wake cycles, hormone secretion, and immune activity. Brain structures that respond to light and darkness coordinate your circadian rhythm and regulate melatonin production. Melatonin is a hormone. It not only signals the body to prepare for sleep but also plays a role in the immune system.

When your natural circadian rhythm is disrupted, it can affect your immune system and cellular functions. During circadian rhythm sleep disorders, the body’s internal clock is misaligned with the external day–night cycle. This can happen due to:
- Irregular sleep schedules
- Shift work
- Frequent hospitalizations
- Reduced exposure to natural light
When your circadian rhythm is disrupted, your hormone cycles and sleep timing are disrupted, too. This can make it difficult to fall asleep at normal times, causing you to wake up too early or to wake up often throughout the night. Over time, circadian disruption can affect your mood, how well your immune system works, and your overall health.
Improving your sleep hygiene can help. Sleep hygiene refers to your sleep habits. You can limit light exposure at night, avoid using screens close to bedtime, and gradually adjust your sleep and wake times. Timed light exposure, like bright light therapy, in the morning can help. Melatonin supplements may be used at carefully timed intervals to help shift circadian rhythms.
Why disrupted sleep can worsen fatigue, pain, and mood
Sleep problems are often part of a symptom cluster in cancer that includes:
- Fatigue
- Pain
- Depression
When sleep is interrupted or shortened, you are less alert during the day. You may feel more distracted and experience fatigue. This can create a cycle that makes it difficult to get good sleep. Your low energy reduces activity levels, which makes it more difficult to sleep well at night.
Poor sleep can also make inflammation worse. This can make you more sensitive to pain and worsen mood symptoms. A study of people with cancer-related fatigue found that a good sleep schedule improved symptoms.
Why do people with cancer have sleep problems?
Sleep problems happen for many different reasons across all phases of cancer care, including before treatment begins, during active therapy, and into survivorship.
Sleep problems in cancer patients often develop from a combination of physical symptoms, emotional stress, biological changes, and environmental changes. These factors can also overlap.
The most common causes of sleep disorders for people with cancer include:
- Physical discomfort and pain. Neuropathy, surgical recovery, bone pain, or treatment side effects can make it difficult to fall or stay asleep.
- Anxiety, depression, and fear. Worry about diagnosis, treatment decisions, or the future can keep the mind alert at night and interfere with relaxation.
- Hormonal changes and inflammation. Cancer and certain treatments can disrupt hormone balance and increase inflammatory activity, affecting circadian rhythm and sleep regulation.
- Hospital stays and nighttime interruptions. Frequent vital sign checks, medications, alarms, and unfamiliar environments can fragment sleep.
- Changes in daily routine and activity levels. Reduced physical activity, increased daytime napping, or extended time in bed can weaken the body’s natural sleep–wake cycle.
- Medications. The use of some anti-cancer therapies may interfere with the sleep schedule and quality.

How do cancer treatments affect sleep?
Cancer treatments can affect sleep in different ways depending on how they interact with the body, immune system, hormones, and nervous system.
Some treatments directly disrupt sleep cycles. Others worsen symptoms like pain, fatigue, or inflammation that interfere with rest. Understanding these effects can help you anticipate changes and work with your care team to protect your sleep quality during treatment.
Chemotherapy
Chemotherapy causes many different side effects, such as nausea, pain, neuropathy, night sweats, or gastrointestinal upset, that can make it hard to stay asleep. Chemotherapy can also increase inflammation and alter circadian rhythms, leading to fragmented sleep or insomnia. It can also cause anxiety surrounding treatment cycles that further disrupt nighttime rest.
Radiation therapy
Radiation therapy is commonly associated with significant fatigue. But this fatigue does not always make it easy to get restful sleep. You may feel exhausted during the day but struggle with nighttime insomnia.
Radiation can also irritate nearby tissues, causing discomfort or inflammation that makes it hard to fall asleep or stay asleep. Over time, disrupted sleep may intensify the cycle of daytime fatigue and nighttime wakefulness.
Immunotherapy
Immunotherapy works by stimulating the immune system to recognize and attack cancer cells. However, this immune activation can increase inflammatory signaling in the body.
Elevated inflammation has been linked to changes in sleep patterns. It can cause increased nighttime awakenings and excessive daytime sleepiness. Flu-like side effects such as fever, chills, or body aches may also temporarily disrupt sleep.
Surgery
Surgery can significantly alter sleep patterns, especially in the immediate recovery period. Pain, limited mobility, hospital monitoring, and anesthesia effects can interrupt sleep. Inflammation and stress responses after surgery may also disrupt circadian rhythms. Some patients have temporary changes in sleep depth and REM sleep as the body recovers from surgical stress.
Steroids and stimulant effects on sleep
Corticosteroids like dexamethasone are commonly used to reduce inflammation, prevent nausea, or manage treatment side effects. These medications can also strongly affect sleep. The body produces a corticosteroid hormone during sleep called cortisol.
When a corticosteroid is used, it may increase alertness, elevate heart rate, and raise energy levels, particularly when taken later in the day. As a result, patients may have difficulty falling asleep, frequent awakenings, or a feeling of being “wired but tired.” If any of these side effects happen to you after taking one of these treatments, talk to your doctor and see if adjusting timing or dosing can help reduce these effects.
Sleep changes during treatment are common and do not mean something is “wrong.” Recognizing these patterns early allows patients and providers to take proactive steps to protect rest, energy, and overall well-being.
What are the different types of sleep disorders?
Sleep disorders are medical conditions that disrupt the ability to fall asleep, stay asleep, or obtain restorative sleep. They can affect any part of the sleep cycle, including the duration and schedule of your sleep, how well you breathe during sleep, how much you move during sleep, and your overall sleep quality.
These problems can lead to fatigue, mood changes, thinking and memory problems, and reduced physical functioning.
Insomnia
Insomnia is the most common sleep disorder. It involves ongoing problems:
- Falling asleep
- Staying asleep
- Waking too early
- Being unable to fall back asleep
Insomnia can be short-term or long-term. Long-term insomnia lasts three months or longer.
Insomnia often leads to fatigue, irritability, difficulty concentrating, and emotional distress. In people undergoing cancer treatment, insomnia may be triggered by anxiety, pain, hospital routines, corticosteroids, or changes in daily schedule.
The first-line treatment for chronic insomnia is cognitive behavioral therapy for insomnia (CBT-I). This is a type of therapy that focuses on understanding thoughts and behaviors around sleep.
Short-term use of sleep medications may be considered during acute stress or medical treatment, but behavioral therapy remains the most effective long-term strategy.
Sleep apnea
Sleep apnea is a breathing-related sleep disorder. During sleep apnea, airflow repeatedly stops and starts during sleep. The most common type is obstructive sleep apnea. It happens when throat muscles relax and block the airway. These pauses in breathing reduce oxygen levels and briefly wake the brain multiple times per hour, even if the person does not remember waking.
Symptoms include:
- Loud snoring.
- Gasping during sleep.
- Morning headaches.
- Excessive daytime sleepiness.
Untreated sleep apnea can increase the risk of cardiovascular problems and worsen fatigue. A treatment for sleep apnea is addressing airway obstruction and improving nighttime breathing.
The most common and effective treatment is continuous positive airway pressure (CPAP), a device that keeps the airway open by delivering steady air pressure through a mask.

Other options include oral appliances fitted by dental specialists, weight management, and positional therapy. In some cases, surgery may be recommended. Treating sleep apnea often improves daytime energy, cardiovascular health, and cognitive function.
Restless legs syndrome (RLS)
Restless legs syndrome is a neurological condition. It is characterized by an uncomfortable urge to move the legs, usually in the evening or at night. People often describe sensations such as tingling, crawling, or pulling that improve with movement. Because symptoms worsen during rest, RLS can make it harder to fall asleep and cause you to wake up frequently. Iron deficiency, nerve damage, or certain medications can contribute to symptoms.
Treatment for RLS focuses on relieving uncomfortable sensations so you can stay asleep. Ways to treat RLS include:
- Fixing iron deficiency when present.
- Reducing caffeine and alcohol intake
- Maintaining regular sleep schedules.
- Moderate exercise and leg stretching may also help.
In moderate to severe cases, medications such as dopamine agonists, gabapentin, or other nerve-calming agents may be prescribed to reduce symptoms.
Excessive daytime sleepiness and cancer-related fatigue
Excessive daytime sleepiness refers to persistent drowsiness and an inability to stay awake during normal waking hours, often caused by poor-quality nighttime sleep or underlying sleep disorders.
Cancer-related fatigue, while sometimes overlapping, is a distinct and often more intense exhaustion. It is not fully relieved by rest. It may be driven by inflammation, anemia, treatment side effects, emotional stress, and disrupted sleep.
Treatment depends on what is causing your sleep problems. If excessive sleepiness is due to sleep apnea, insomnia, or medication side effects, addressing those conditions can significantly improve alertness. Cancer-related fatigue may require a multifaceted approach, including:
- Managing anemia
- Controlling pain
- Engaging in light physical activity
- Improving nighttime sleep quality
- Addressing emotional distress.
- Energy conservation strategies
- Structured daytime activity
How are sleep disorders diagnosed?
Sleep disorders are diagnosed through a combination of health history, symptom questionnaires, sleep diaries, and sometimes specialized testing. A diagnosis can help find the best therapy to improve your quality of life.
A healthcare provider will ask about sleep patterns, daytime symptoms, medical history, and medications. You may be asked to track sleep habits for several weeks. You may have a specialized test called the polysomnography. This is an overnight sleep study that helps identify sleep cycles and breathing patterns during sleep. Another option if sleep apnea is suspected is a home sleep apnea test. This can be done to monitor breathing, oxygen levels, heart rate, and brain activity during sleep.

What are natural ways to improve sleep quality?
There are medications that can help you sleep, but they do have some risks. These include a risk of dependency and thinking and memory (cognitive) problems. Before using sleep medications, your healthcare team will help you try other approaches. Changing your habits is often the most effective long-term solution for treating sleep disorders, especially insomnia.
Non-medical therapies focus on retraining the brain and body to associate the bed with sleep, regulating the circadian rhythm, and reducing physical and emotional stimuli at night. Unlike medications, behavioral strategies address the root causes of your sleep problems. They can provide lasting improvement. Below are evidence-based approaches without medication that can significantly improve sleep quality.
Cognitive behavioral therapy for insomnia (CBT-I)
CBT-I is considered the gold standard treatment for chronic insomnia. It helps identify and change thoughts and behaviors that interfere with sleep. CBT-I often includes:
- Stimulus control. This technique helps people with insomnia change negative associations they may have with the bed and the bedroom.
- Sleep restriction therapy. This is changing sleep so it happens in a consistent window. Cognitive restructuring. This is identifying and challenging negative beliefs and anxious thoughts about sleep.
- Relaxation training.
CBT-I is highly effective and produces durable results without medication side effects.This therapy needs professional counseling and commitment to slowly make permanent changes in habits with the purpose of getting used to these new habits and sleeping better.
Relaxation techniques and mindfulness
Stress is one of the main causes of insomnia. Relaxation practices such as progressive muscle relaxation, guided imagery, body scans, and mindfulness meditation help calm the nervous system before bedtime. These techniques reduce cortisol levels, slow heart rate, and create the mental shift necessary for sleep onset.
Methods such as diaphragmatic breathing or slow breathing techniques can lower heart rate and reduce anxiety at bedtime. Breathing exercises are simple, portable tools that can be used during nighttime awakenings as well.
Physical activity can help regulate your sleep schedule
Light physical activity during the day helps you fall asleep and improves overall sleep quality. Gentle evening stretching, restorative yoga, or slow mobility exercises can help release muscle tension and reduce discomfort. Regular daytime exercise can support deeper sleep, though vigorous workouts close to bedtime may be stimulating for some people.
Regulating the circadian rhythm with light
Light is the most powerful regulator of the body’s internal clock. Morning exposure to natural sunlight helps signal wakefulness and strengthens circadian alignment. In contrast, limiting bright light and screen exposure in the evening supports melatonin production. For people with circadian rhythm disruptions, structured light exposure and consistent wake times are especially important for stabilizing sleep patterns.
For example, new devices such as sunrise alarms can help regulate the circadian cycle with only light therapy.
What is sleep hygiene? How a good nighttime sleep routine can be life-changing
Sleep hygiene refers to daily habits and environmental practices that promote restorative sleep. While sleep hygiene alone may not cure chronic insomnia, it forms the foundation for healthy sleep. Over time, consistency strengthens the brain’s association between bed and rest.
The tips below can help you improve your sleep hygiene and get better, more restful sleep.
Create a cozy environment in your bedroom
- Keep the bedroom cool, dark, and quiet to help your body wind down.
- Choose a comfortable mattress, pillows, and bedding that support restful sleep.
- Reserve your bed for sleep only, not work or TV, so your brain associates it with rest.
Adhere to a consistent bedtime
- Go to sleep and wake up at the same times every day, even weekends.
- Avoid long or late naps that can make it harder to fall asleep at night.
Prepare your body for sleeping
- Wind down with relaxing activities before bed, such as reading, gentle stretching, or listening to soothing music.
- Disconnect from screens such as phones, tablets, computers, and TVs at least 30 to 60 minutes before bed. This is because blue light from screens can delay melatonin production and keep you awake.
- If you can’t fall asleep after around 20 minutes in bed, get up and do something calming in dim light until you feel sleepy again.
Small daily habits make a big difference
- Get daylight exposure to help regulate your sleep–wake rhythm.
- Keep active with regular exercise (but avoid intense workouts too close to bedtime).
- Avoid caffeine and alcohol in the hours before sleep, and avoid heavy meals close to bedtime.
Is napping helpful or harmful?
Napping can be helpful if done at the right time and for the right duration. Short naps between 20 and 30 minutes earlier in the day may improve alertness without interfering with nighttime sleep. For those experiencing cancer-related fatigue, carefully timed brief naps may support energy while preserving nighttime rest.
However, napping for too long or too late during the day can further affect sleep disorders, making it harder to fall asleep at night. For people struggling with insomnia, limiting or eliminating daytime naps is often recommended.
When should you talk to your healthcare team about sleep?
Sleep problems are common during and after cancer treatment, but persistent or severe disturbances should not be ignored. Research shows that sleep disruption can worsen fatigue, mood changes, pain perception, and overall quality of life , and may also be linked to immune and inflammatory changes. Because sleep plays a role in recovery and treatment tolerance, discussing concerns early allows for proper evaluation and targeted support.
You should always talk to your healthcare team about sleep problems, even if they seem minor.
There are some signs that your sleep problems might be more serious. Talk to your health care team right away if you experience:
- Difficulty falling or staying asleep three or more nights per week
- Loud snoring, gasping, or pauses in breathing during sleep
- Persistent daytime sleepiness that interferes with daily functioning
- Severe fatigue that does not improve with rest
- Restless, uncomfortable sensations in the legs at night
- Mood changes (increased anxiety, irritability, or depression) linked to poor sleep
- Sleep disruption that continues for weeks or worsens during treatment
These signs may indicate insomnia, sleep apnea, restless legs syndrome, circadian rhythm disruption, or treatment-related sleep changes that require medical attention.
What to ask your care team
Open communication can lead to better and faster solutions. Clearing your questions with your healthcare team can help them analyze what may be interfering with your rest.
- Could my treatment or medications be affecting my sleep?
- Should I be evaluated for a sleep disorder?
- Would cognitive behavioral therapy for insomnia (CBT-I) help me?
- Are there safe sleep aids or alternatives I can use?
- Could my fatigue be related to a sleep problem rather than just treatment?
Keep in mind that before self-medicating with sleep medications, there are many changes that don’t require medication and are proven effective against sleep disorders. Always ask your team before considering a new medication, and keep open communication with your loved ones to provide better support with daily routines around bedtime.
Sleep is a biologically essential process. It supports immune regulation, tissue repair, emotional balance, cognitive function, and overall resilience. Throughout this article, we’ve explored how sleep cycles restore the body and brain, how cancer and its treatments can disrupt normal sleep patterns, and how untreated sleep problems can worsen fatigue, pain, mood changes, and quality of life.
If you are struggling with sleep, don’t wait. Bring it up at your next appointment. Sleep problems are common during cancer care, and they are treatable. Ask your healthcare team about screening for sleep disorders, behavioral therapies like CBT-I, or strategies to improve your sleep routine.
Visit HealthTree’s Side Effect Solutions to see what has worked for others or create an account to contribute with what has worked for you!
CREATE YOUR HEALTHTREE ACCOUNT
Sources:
- Good Sleep for Good Health
- Sleep duration and the risk of cancer: a systematic review and meta-analysis including dose–response relationship
- The Triad of Sleep, Immunity, and Cancer: A Mediating Perspective
- Sleep disorders and cancer: State of the art and future perspectives
- Sleep/Wake Disturbances in People With Cancer and Their Caregivers: State of the Science
- Physiology, Sleep Stages
- Why Is Sleep Important?

about the author
Jimena Vicencio
Jimena is an International Medical Graduate and a member of the HealthTree Writing team. Currently pursuing a bachelor's degree in journalism, she combines her medical background with a storyteller’s heart to make complex healthcare topics accessible to everyone. Driven by a deep belief that understanding health is a universal right, she is committed to translating scientific and medical knowledge into clear, compassionate language that empowers individuals to take control of their well-being.
More on Navigating Your Health
Trending Articles
Get the Latest Angioimmunoblastic T-Cell Lymphoma Updates, Delivered to You.
By subscribing to the HealthTree newsletter, you'll receive the latest research, treatment updates, and expert insights to help you navigate your health.
Together we care.
Together we cure.









