What is Polypharmacy? Managing Your Medications When You Have Cancer

Many people diagnosed with cancer are already managing pre-existing conditions like heart disease, high blood pressure, or diabetes. These conditions often require medication.
Once an oncologist creates a treatment plan, the list of medications you are taking grows. Patients often begin taking targeted oral therapies and corticosteroids, like dexamethasone, alongside supportive care medications to manage side effects like nausea, bone pain, or digestive issues. When a person takes five or more medications daily, it is called polypharmacy.
In the past, polypharmacy was seen simply as a "warning sign" to check for drug errors. However, recent research has shown that managing this list needs to be a priority, especially for people with cancer. There is a link between high pill counts and lower survival rates and an increased risk of severe infections.
The risk is often highest when communication gaps exist between different medical teams. For instance, if a primary care doctor prescribes acetaminophen for pain and an oncologist suggests Tylenol for a fever, a patient may accidentally take a double dose because they don't realize it is the same drug. This is why a medication review is so vital. By mindfully adjusting these prescriptions, your care team can reduce your daily pill burden. This is a process known as deprescribing. It can prevent dangerous interactions and significantly improve your overall quality of life.
The risk of taking many medications relies on how they interact inside the body
Sometimes, medications can have negative effects when taken together. This is called a drug interaction. When you are managing chronic diseases like diabetes, hypertension, or heart disease, your care team needs to know your treatment plan. That way they can see how the medications for any chronic conditions and the cancer will interact with each other.
The risk of a drug interaction increases with every new medication. This is even true with alternative treatments and supplements. This is why having an open line of communication with your healthcare team is crucial. They can help double-check if you really need supplementation, and if the new medication has a risk of interacting with your baseline treatment. Read more: Can supplements interact with my current medications?
What are drug interactions?
To help you understand how multiple medications can interact in your body, it is useful to look at where and how these interactions happen.
Drug interactions are categorized into three main types:
- Pharmaceutical: based on whether they happen before entering the body
- Pharmacokinetic: during the medication’s pass through your body
- Pharmacodynamic: at the final target site.
Pharmaceutical interactions: the "mixing" phase
These interactions happen before a medication enters your bloodstream. They are often chemical or physical reactions that occur when two drugs are mixed in the same IV bag or syringe. This is usually noted by the health professional administering the medication, who may notice tiny crystals or cloudiness in the liquid.
If this happens, the medication becomes inactive or, in rare cases, can be dangerous to inject.
Some monoclonal antibodies used in blood cancer, like rituximab, are very sensitive to what they are mixed with. If a nurse were to mix certain medications into a bag containing "dextrose" instead of "normal saline", the drug can break down or clump together before it even enters the patient’s arm. This is why oncology nurses are highly trained to never mix certain chemotherapies in the same line.
Pharmacokinetic interactions: the "journey" phase
This is the most common type of interaction in polypharmacy. It describes how one drug changes the way your body handles another. Experts use the acronym ADME to describe this journey.
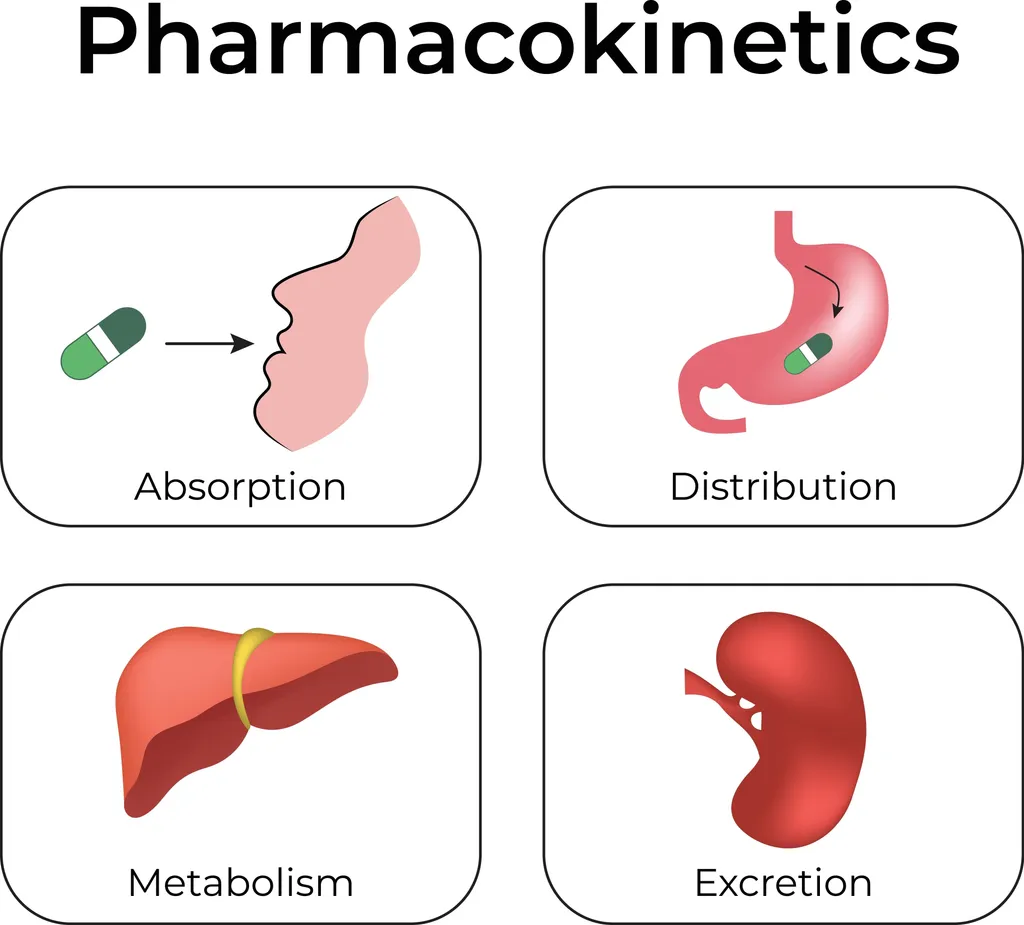
Absorption. Sometimes, one medication can prevent another from entering your blood. For example, taking an antacid can change your stomach’s acidity so much that an oral cancer pill cannot dissolve or be absorbed properly.
Distribution: Medication travels through the blood by “hitching a ride” on proteins. Sometimes, two medications can compete for the same “seat” on a protein. This could increase the concentration of the medication that ends up in the bloodstream. It can cause a delayed effect or even intoxication.
Metabolism: Metabolism is how quickly the body processes medications and other substances. This happens in the liver. Sometimes, this process can be stopped or sped up, making medications work in ways they shouldn’t. For example, St. John’s wort, which is an herbal supplement, can “wake up” liver enzymes. This can impact cancer drugs like ibrutinib (Imbruvica) and affect how they work.
Excretion: This happens in the kidneys. Some medications can block the “exit doors” in your kidneys. This causes other medications to build up in your body and cause toxicity. For example, if the common chemotherapy methotrexate and ibuprofen are taken together, your kidneys will process the ibuprofen first. The methotrexate backs up in your blood. This leads to a life-threatening toxicity because the chemo stays in your blood much longer than it should.
Understanding interactions leaves an important message: even if a medication or supplement is easy to access or sold over the counter, you should always ask your healthcare team if you can take them. By describing your symptoms, it is likely you will encounter a solution that doesn’t risk a drug interaction.
Pharmacodynamic interactions: the "action" phase
Medications can interact at the same spot if taken together or on the same day. There are three ways this happens:
Additive Effect (1 + 1 = 2): Two drugs with similar effects are taken together. While this can be helpful, it can also double your side effects, like two different meds both causing extreme drowsiness.
Synergistic Effect (1 + 1 = 5): The drugs "team up" to create an effect much stronger than either could do alone. In blood cancer, this effect is often used on purpose. For example, combining two chemotherapy treatments. But it becomes a risk when an over-the-counter supplement accidentally supercharges a medication’s toxicity.
Antagonistic Effect (1 + 1 = 0): One drug blocks the other. A common example is taking a "natural" antioxidant supplement that accidentally protects the cancer cells from the chemotherapy meant to kill them.
Before removing or adding a medication or supplement, always ask your healthcare team.Keep a list of all the medications and supplements you take regularly. If you have more than one doctor, keep track of who prescribed them. This way it will be easier for you and your team to confirm there will be no harmful interactions.
Over-the-counter medications and supplements can interact with cancer treatment, too
It is not only prescribed medications that can have harmful effects when combined. Many medications are over-the-counter or even herbal supplements.
Aspirin and NSAIDs. These common pain relievers are helpful for headaches, fever, and pain symptoms. However they can affect platelets. If you have low platelet counts, taking aspirin on a regular basis can have a blood thinning effect. This can also aggravate stomach ulcers.
A risk for many cancer patients is that these medications may hide fever that could aggravate into a serious infection. In many cases acetaminophen (Tylenol) is usually the "safe" choice, but requires dose monitoring for liver safety.
Proton pump inhibitors like Prilosec, Nexium). These medications can alter the gut microbiome. This can reduce the absorption of some medications by altering the stomach’s pH. They can potentially reduce the effectiveness of Immunotherapy and other oral chemotherapies.
Herbal supplements such as turmeric & St. John’s wort These common supplements can interfere with targeted therapies like imatinib (Gleevec) by speeding up liver metabolism. This essentially flushes the cancer drug out too fast. Complementary medicine can be incorporated into your care, but it is important to do so safely.
Sleep and insomnia medications. Some of these medications increase the risk of cognitive impairment, delirium, and dangerous physical falls. Common antihistamines used for sleep are also risky, as they can cause confusion. Sleep problems can be challenging. It’s important to talk to your care team if you are having trouble sleeping.
How common are problems caused by polypharmacy according to real-world data?
The number of prescriptions a person has is the strongest predictor of if someone will experience a harmful medication event.
A study of 82 million patients from 2007 to 2014 in the United States, analyzed how people use multiple medications. The data shows that:
- 10% of the U.S. population and 30% of older adults take 5 or more drugs at the same time.
- Among those taking any prescription, 50% are using 2 or more drugs, and 5% are using 8 or more.
- Adverse drug reactions cause 4 hospitalizations per 1,000 people every year.
- Over 20% of adverse reactions that end up in hospitalizations are caused by drug-drug interaction
- The study identified 220 million unique drug-ingredient combinations.
Specific three-drug combinations, such as mixing acetaminophen (Tylenol) and oxycodone (Endone/OxyContin) with the nausea medication prochlorperazine (Compazine), are associated with emergency department visit rates 3.6 times higher than the general population.
How to recognize the red flags of a possible drug-interaction?
While understanding the science of drug interactions is helpful, it is even more important to recognize when your body is alerting you that something is wrong.
Because some cancer treatments can lower your protective white blood cells and platelets, small symptoms can quickly become serious.
- Fever: If your temperature reaches 100.4°F (38°C) or higher, contact your oncology team right away. Do not take over-the-counter cold medicine to lower the fever. This can "mask" a serious infection and delay life-saving care.
- Unusual bleeding or bruising: Look for tiny, pinpoint red spots on the skin (petechiae) or bruises that appear without an injury. This is a sign that a medication, like an NSAID, is interfering with your already low platelet count.
- Sudden confusion or dizziness: Many medications can affect the central nervous system. If you or a loved one experiences a sudden change in balance or mental clarity, it may be a sign of a "drug-to-drug" collision.
- Rapid glucose changes: If you are taking corticosteroids (such as dexamethasone) as part of your treatment, be alert for sudden spikes in blood sugar, which can be triggered by "hidden" sugars in liquid cough syrups or interactions with other medications. Some signs of blood sugar spikes can be feeling sleepy or drowsy after sugary meals, headache, confusion, and extreme thirst.
The role of pharmacists
In cancer care, pharmacists are a vital part of your health team. An oncopharmacist is specifically trained to manage medications for people with cancer and bridge communication gaps among doctors.
- Medication reconciliation: This is a process in which the pharmacist reviews your entire list to ensure that "Drug A" from your cardiologist doesn't interact with "Drug B" from your hematologist.
- Safety screening: Pharmacists use advanced databases to identify high-risk combinations. For example, they can flag 3-drug combinations (like certain pain and nausea meds) that are known to increase emergency room visits by 3.6 times.
- The "one pharmacy" rule: To keep you safe, try to fill all prescriptions at a single pharmacy. This allows their computer system to automatically alert the pharmacist if a new prescription is a poor match for your current medications.
How can I prevent drug interactions in my care?
As a patient you are not obligated to understand all drug interactions. The medical professionals prescribing them to you have that responsibility. However, you can take an active role in preventing polypharmacy by following simple habits:
- Keep a journal or detailed notes: Write or keep track of what has been prescribed to you in a journal or app. Include the date you started taking them, frequency, time of day you take them, and how you feel after taking them. This will help you identify possible side effects.
- Ask your care team to do a “brown bag review.” This is very simple: you place every single medication, vitamin, and herbal supplement you take into a bag and bring it to your appointment for a physical review. This way, your team will ensure you are not taking duplicate medications or risking interactions.
- Centralize your records: Use a digital health tool, like HealthTree, to keep your full medical history and medication list in one place. This ensures that no matter which specialist you see, they have the same accurate information.
Create your free HealthTree account and securely connect your records to keep track of your health journey all in one place!
Questions to ask your care team
- Does this new over-the-counter medication affect my specific chemotherapy or immunotherapy?
- Are there any baseline medications I am currently taking for other conditions that we can safely reduce or stop (deprescribing)?
- Which pain or cold medications are the safest for me to use if my platelet or white blood cell counts are low?
- Should I be avoiding any specific foods, like grapefruit, while on this treatment?
- Can you provide a 'safe swap' list for common symptoms like congestion or sleep issues?
Source:
- Association of Polypharmacy and Potentially Inappropriate Medications With Frailty Among Older Adults With Blood Cancers
- Polypharmacy independently predicts survival, hospitalization, and infections in patients with lymphoid cancer
- American Geriatrics Society 2023 updated AGS Beers Criteria® for potentially inappropriate medication use in older adults
- A dataset quantifying polypharmacy in the United States
- Practical Pharmacokinetic–Pharmacodynamic Models in Oncology
- Polypharmacy
Many people diagnosed with cancer are already managing pre-existing conditions like heart disease, high blood pressure, or diabetes. These conditions often require medication.
Once an oncologist creates a treatment plan, the list of medications you are taking grows. Patients often begin taking targeted oral therapies and corticosteroids, like dexamethasone, alongside supportive care medications to manage side effects like nausea, bone pain, or digestive issues. When a person takes five or more medications daily, it is called polypharmacy.
In the past, polypharmacy was seen simply as a "warning sign" to check for drug errors. However, recent research has shown that managing this list needs to be a priority, especially for people with cancer. There is a link between high pill counts and lower survival rates and an increased risk of severe infections.
The risk is often highest when communication gaps exist between different medical teams. For instance, if a primary care doctor prescribes acetaminophen for pain and an oncologist suggests Tylenol for a fever, a patient may accidentally take a double dose because they don't realize it is the same drug. This is why a medication review is so vital. By mindfully adjusting these prescriptions, your care team can reduce your daily pill burden. This is a process known as deprescribing. It can prevent dangerous interactions and significantly improve your overall quality of life.
The risk of taking many medications relies on how they interact inside the body
Sometimes, medications can have negative effects when taken together. This is called a drug interaction. When you are managing chronic diseases like diabetes, hypertension, or heart disease, your care team needs to know your treatment plan. That way they can see how the medications for any chronic conditions and the cancer will interact with each other.
The risk of a drug interaction increases with every new medication. This is even true with alternative treatments and supplements. This is why having an open line of communication with your healthcare team is crucial. They can help double-check if you really need supplementation, and if the new medication has a risk of interacting with your baseline treatment. Read more: Can supplements interact with my current medications?
What are drug interactions?
To help you understand how multiple medications can interact in your body, it is useful to look at where and how these interactions happen.
Drug interactions are categorized into three main types:
- Pharmaceutical: based on whether they happen before entering the body
- Pharmacokinetic: during the medication’s pass through your body
- Pharmacodynamic: at the final target site.
Pharmaceutical interactions: the "mixing" phase
These interactions happen before a medication enters your bloodstream. They are often chemical or physical reactions that occur when two drugs are mixed in the same IV bag or syringe. This is usually noted by the health professional administering the medication, who may notice tiny crystals or cloudiness in the liquid.
If this happens, the medication becomes inactive or, in rare cases, can be dangerous to inject.
Some monoclonal antibodies used in blood cancer, like rituximab, are very sensitive to what they are mixed with. If a nurse were to mix certain medications into a bag containing "dextrose" instead of "normal saline", the drug can break down or clump together before it even enters the patient’s arm. This is why oncology nurses are highly trained to never mix certain chemotherapies in the same line.
Pharmacokinetic interactions: the "journey" phase
This is the most common type of interaction in polypharmacy. It describes how one drug changes the way your body handles another. Experts use the acronym ADME to describe this journey.

Absorption. Sometimes, one medication can prevent another from entering your blood. For example, taking an antacid can change your stomach’s acidity so much that an oral cancer pill cannot dissolve or be absorbed properly.
Distribution: Medication travels through the blood by “hitching a ride” on proteins. Sometimes, two medications can compete for the same “seat” on a protein. This could increase the concentration of the medication that ends up in the bloodstream. It can cause a delayed effect or even intoxication.
Metabolism: Metabolism is how quickly the body processes medications and other substances. This happens in the liver. Sometimes, this process can be stopped or sped up, making medications work in ways they shouldn’t. For example, St. John’s wort, which is an herbal supplement, can “wake up” liver enzymes. This can impact cancer drugs like ibrutinib (Imbruvica) and affect how they work.
Excretion: This happens in the kidneys. Some medications can block the “exit doors” in your kidneys. This causes other medications to build up in your body and cause toxicity. For example, if the common chemotherapy methotrexate and ibuprofen are taken together, your kidneys will process the ibuprofen first. The methotrexate backs up in your blood. This leads to a life-threatening toxicity because the chemo stays in your blood much longer than it should.
Understanding interactions leaves an important message: even if a medication or supplement is easy to access or sold over the counter, you should always ask your healthcare team if you can take them. By describing your symptoms, it is likely you will encounter a solution that doesn’t risk a drug interaction.
Pharmacodynamic interactions: the "action" phase
Medications can interact at the same spot if taken together or on the same day. There are three ways this happens:
Additive Effect (1 + 1 = 2): Two drugs with similar effects are taken together. While this can be helpful, it can also double your side effects, like two different meds both causing extreme drowsiness.
Synergistic Effect (1 + 1 = 5): The drugs "team up" to create an effect much stronger than either could do alone. In blood cancer, this effect is often used on purpose. For example, combining two chemotherapy treatments. But it becomes a risk when an over-the-counter supplement accidentally supercharges a medication’s toxicity.
Antagonistic Effect (1 + 1 = 0): One drug blocks the other. A common example is taking a "natural" antioxidant supplement that accidentally protects the cancer cells from the chemotherapy meant to kill them.
Before removing or adding a medication or supplement, always ask your healthcare team.Keep a list of all the medications and supplements you take regularly. If you have more than one doctor, keep track of who prescribed them. This way it will be easier for you and your team to confirm there will be no harmful interactions.
Over-the-counter medications and supplements can interact with cancer treatment, too
It is not only prescribed medications that can have harmful effects when combined. Many medications are over-the-counter or even herbal supplements.
Aspirin and NSAIDs. These common pain relievers are helpful for headaches, fever, and pain symptoms. However they can affect platelets. If you have low platelet counts, taking aspirin on a regular basis can have a blood thinning effect. This can also aggravate stomach ulcers.
A risk for many cancer patients is that these medications may hide fever that could aggravate into a serious infection. In many cases acetaminophen (Tylenol) is usually the "safe" choice, but requires dose monitoring for liver safety.
Proton pump inhibitors like Prilosec, Nexium). These medications can alter the gut microbiome. This can reduce the absorption of some medications by altering the stomach’s pH. They can potentially reduce the effectiveness of Immunotherapy and other oral chemotherapies.
Herbal supplements such as turmeric & St. John’s wort These common supplements can interfere with targeted therapies like imatinib (Gleevec) by speeding up liver metabolism. This essentially flushes the cancer drug out too fast. Complementary medicine can be incorporated into your care, but it is important to do so safely.
Sleep and insomnia medications. Some of these medications increase the risk of cognitive impairment, delirium, and dangerous physical falls. Common antihistamines used for sleep are also risky, as they can cause confusion. Sleep problems can be challenging. It’s important to talk to your care team if you are having trouble sleeping.
How common are problems caused by polypharmacy according to real-world data?
The number of prescriptions a person has is the strongest predictor of if someone will experience a harmful medication event.
A study of 82 million patients from 2007 to 2014 in the United States, analyzed how people use multiple medications. The data shows that:
- 10% of the U.S. population and 30% of older adults take 5 or more drugs at the same time.
- Among those taking any prescription, 50% are using 2 or more drugs, and 5% are using 8 or more.
- Adverse drug reactions cause 4 hospitalizations per 1,000 people every year.
- Over 20% of adverse reactions that end up in hospitalizations are caused by drug-drug interaction
- The study identified 220 million unique drug-ingredient combinations.
Specific three-drug combinations, such as mixing acetaminophen (Tylenol) and oxycodone (Endone/OxyContin) with the nausea medication prochlorperazine (Compazine), are associated with emergency department visit rates 3.6 times higher than the general population.
How to recognize the red flags of a possible drug-interaction?
While understanding the science of drug interactions is helpful, it is even more important to recognize when your body is alerting you that something is wrong.
Because some cancer treatments can lower your protective white blood cells and platelets, small symptoms can quickly become serious.
- Fever: If your temperature reaches 100.4°F (38°C) or higher, contact your oncology team right away. Do not take over-the-counter cold medicine to lower the fever. This can "mask" a serious infection and delay life-saving care.
- Unusual bleeding or bruising: Look for tiny, pinpoint red spots on the skin (petechiae) or bruises that appear without an injury. This is a sign that a medication, like an NSAID, is interfering with your already low platelet count.
- Sudden confusion or dizziness: Many medications can affect the central nervous system. If you or a loved one experiences a sudden change in balance or mental clarity, it may be a sign of a "drug-to-drug" collision.
- Rapid glucose changes: If you are taking corticosteroids (such as dexamethasone) as part of your treatment, be alert for sudden spikes in blood sugar, which can be triggered by "hidden" sugars in liquid cough syrups or interactions with other medications. Some signs of blood sugar spikes can be feeling sleepy or drowsy after sugary meals, headache, confusion, and extreme thirst.
The role of pharmacists
In cancer care, pharmacists are a vital part of your health team. An oncopharmacist is specifically trained to manage medications for people with cancer and bridge communication gaps among doctors.
- Medication reconciliation: This is a process in which the pharmacist reviews your entire list to ensure that "Drug A" from your cardiologist doesn't interact with "Drug B" from your hematologist.
- Safety screening: Pharmacists use advanced databases to identify high-risk combinations. For example, they can flag 3-drug combinations (like certain pain and nausea meds) that are known to increase emergency room visits by 3.6 times.
- The "one pharmacy" rule: To keep you safe, try to fill all prescriptions at a single pharmacy. This allows their computer system to automatically alert the pharmacist if a new prescription is a poor match for your current medications.
How can I prevent drug interactions in my care?
As a patient you are not obligated to understand all drug interactions. The medical professionals prescribing them to you have that responsibility. However, you can take an active role in preventing polypharmacy by following simple habits:
- Keep a journal or detailed notes: Write or keep track of what has been prescribed to you in a journal or app. Include the date you started taking them, frequency, time of day you take them, and how you feel after taking them. This will help you identify possible side effects.
- Ask your care team to do a “brown bag review.” This is very simple: you place every single medication, vitamin, and herbal supplement you take into a bag and bring it to your appointment for a physical review. This way, your team will ensure you are not taking duplicate medications or risking interactions.
- Centralize your records: Use a digital health tool, like HealthTree, to keep your full medical history and medication list in one place. This ensures that no matter which specialist you see, they have the same accurate information.
Create your free HealthTree account and securely connect your records to keep track of your health journey all in one place!
Questions to ask your care team
- Does this new over-the-counter medication affect my specific chemotherapy or immunotherapy?
- Are there any baseline medications I am currently taking for other conditions that we can safely reduce or stop (deprescribing)?
- Which pain or cold medications are the safest for me to use if my platelet or white blood cell counts are low?
- Should I be avoiding any specific foods, like grapefruit, while on this treatment?
- Can you provide a 'safe swap' list for common symptoms like congestion or sleep issues?
Source:
- Association of Polypharmacy and Potentially Inappropriate Medications With Frailty Among Older Adults With Blood Cancers
- Polypharmacy independently predicts survival, hospitalization, and infections in patients with lymphoid cancer
- American Geriatrics Society 2023 updated AGS Beers Criteria® for potentially inappropriate medication use in older adults
- A dataset quantifying polypharmacy in the United States
- Practical Pharmacokinetic–Pharmacodynamic Models in Oncology
- Polypharmacy

about the author
Jimena Vicencio
Jimena is an International Medical Graduate and a member of the HealthTree Writing team. Currently pursuing a bachelor's degree in journalism, she combines her medical background with a storyteller’s heart to make complex healthcare topics accessible to everyone. Driven by a deep belief that understanding health is a universal right, she is committed to translating scientific and medical knowledge into clear, compassionate language that empowers individuals to take control of their well-being.
More on Navigating Your Health
Trending Articles
Get the Latest Blood Cancer Updates, Delivered to You.
By subscribing to the HealthTree newsletter, you'll receive the latest research, treatment updates, and expert insights to help you navigate your health.
Together we care.
Together we cure.













