Understanding Prostate Cancer
What is Prostate Cancer?
Last updated and reviewed on March 19, 2026.
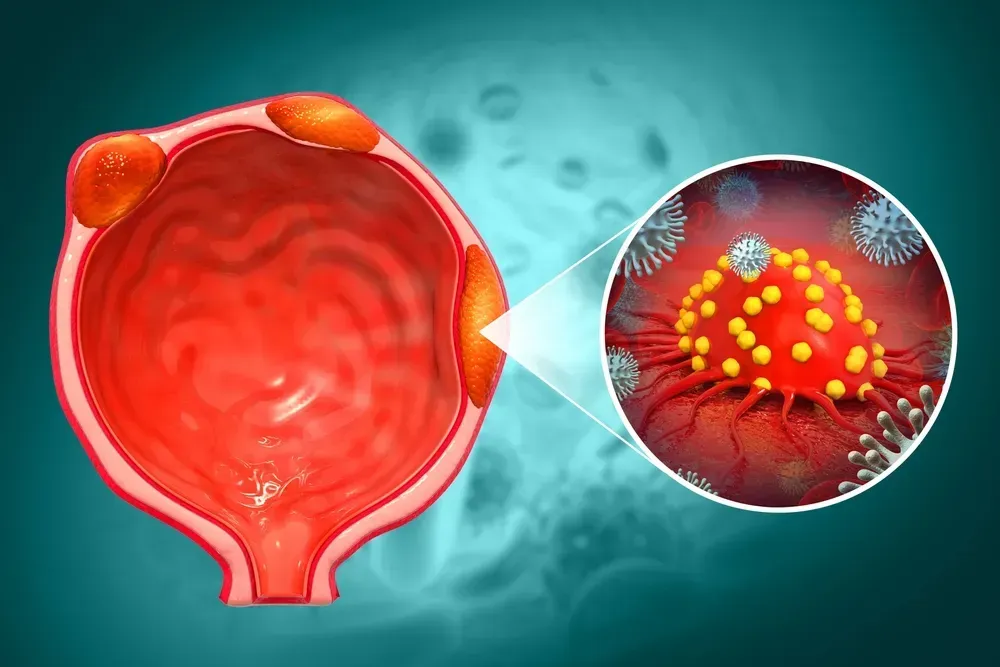
Cancer begins when cells grow out of control. Prostate cancer affects the prostate gland. When you have prostate cancer, cells in the prostate do not follow the normal cell cycle. Normal cells grow, replicate (copy themselves), and then die. Cancer cells change, grow faster than normal, replicate too fast, and do not die as they should.
How does prostate cancer affect the prostate?
|
THE BASICS: When you have prostate cancer, your prostate cells grow too quickly and form a tumor. Prostate cancer is one of the most common cancers in men. It is also one of the most treatable, especially when caught early. Most men are diagnosed with prostate cancer at the localized stage. This means it has not spread to other parts of the body. |
Sometimes, prostate cancer can spread to other parts of the body. Around 1 in 4 men diagnosed with prostate cancer have more advanced disease at the time of diagnosis. Prostate cancer most often spreads to the bones (80%), lymph nodes (10%), liver (10%), and the lungs (9%)2. The good news is that prostate cancer often grows very slowly. Many men with early-stage prostate cancer live normal lives without needing immediate treatment. Doctors use a blood test called a PSA Test, along with imaging and biopsies, to detect and monitor it. When it does require treatment, prostate cancer treatment is often very successful, even for people with more advanced cancer.
What is the Prostate?
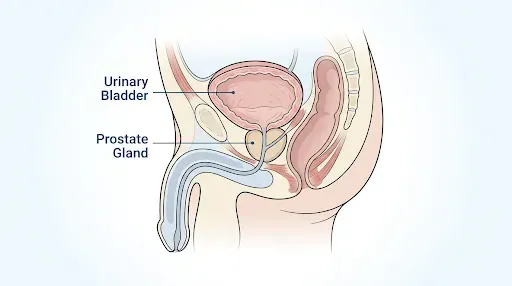
The prostate is a small gland, about the size of a walnut. It is located directly below the bladder. It surrounds the urethra, which is the tube that carries urine out of the bladder. The prostate gland produces seminal fluid. Together with sperm cells from the testicles and fluids from other glands, this fluid makes up semen.
When a person has prostate cancer, their prostate cells grow too quickly. The extra cells build up and form tumors.
How does prostate cancer affect the body?
In the early stages, prostate cancer usually does not cause pain or noticeable symptoms. The first sign of prostate cancer for many men is high levels of prostate-specific antigen (PSA) on a blood test. PSA is a protein. Small amounts of PSA are normal, but high levels of PSA can be a sign of prostate cancer or another condition affecting the prostate.
As the tumor grows, it can cause:
-
Trouble starting or stopping the flow of urine
A weak or interrupted urine stream
Needing to urinate more often, especially at night
A feeling that the bladder is not fully empty
Blood in the urine or semen
Pain with ejaculation
When prostate cancer spreads to other parts of the body, it most commonly affects the bones, causing pain that may wake you up at night. If it spreads to the spine, it can press on nerves and cause back pain or weakness.
Learn more about the signs and symptoms of Prostate Cancer.
Types of prostate cancer
There are several types of prostate cancer, though one type is by far the most common:
-
Acinar adenocarcinoma. The most common type of prostate cancer. It develops in the glandular cells of the prostate called acini. Acinar adenocarcinoma is what most people mean when they say "prostate cancer."
-
Ductal adenocarcinoma. A less common type that tends to grow and spread more quickly than acinar adenocarcinoma. It also begins in the gland cells of the prostate, but in the ductal cells. Sometimes prostate cancer can have both acinar and ductal cancer cells.
-
Neuroendocrine carcinoma. A rare type that starts in special cells called neuroendocrine cells. Small-cell prostate cancer is the most common form of this type and tends to grow faster than other types.
-
Adenosquamous carcinoma. A very rare type made up of two different kinds of cancer cells.
Sarcoma. A rare type that starts in the muscle tissue of the prostate.
Lymphoma. A very rare type where cancer of the lymph system starts in the prostate. Most of the time, prostate lymphoma is a type of non-Hodgkin lymphoma.
Prostate cancer subtypes
Within those main types, doctors can break prostate cancer down even further into subtypes. There are two ways to look at subtypes:
By How the Cells Look (Histological Subtypes)
When a doctor looks at prostate cancer cells under a microscope, they can sometimes see special patterns that help identify a subtype. Some examples include:
-
Signet-cell-like adenocarcinoma. Cancer cells that look like signet rings under a microscope.
-
Sarcomatoid carcinoma. A rare and aggressive form where cancer cells look like sarcoma cells.
-
Squamous cell carcinoma. A very rare form that develops from flat cells lining the prostate.
Adenoid cystic carcinoma. A very rare, slow-growing subtype that begins in the basal cells of the prostate.
Recognizing these subtypes is important. It can help identify prostate cancer that grows more quickly and help choose treatments.
By the Genes Inside the Cancer Cells (Molecular Subtypes)
Scientists have also found that prostate cancer can be broken down into subtypes based on changes in the genes inside the cancer cells. Think of genes like instructions inside a cell. When those instructions get changed or damaged, cancer can develop.
Some of the most common gene changes found in prostate cancer include:
-
ERG gene fusions. The most common gene change is found in about half of all prostate cancers.
-
SPOP mutations. Found in about 1 in 10 prostate cancers.
-
FOXA1 mutations. A less common gene change.
Understanding the gene changes in a person's prostate cancer is becoming increasingly important. This is because it helps doctors choose the best treatment and predict how the cancer may behave over time.
What are the related disorders to prostate cancer?
The following conditions are not cancer, but they are changes in the prostate cells that doctors watch carefully because they can sometimes lead to cancer. These are sometimes known as precursor conditions or precancerous conditions.
Prostatic Intraepithelial Neoplasia (PIN)
PIN means some of the cells lining the prostate look abnormal under a microscope. Think of it as cells that have started to look "different" but have not yet grown into surrounding tissue. There are two types:
-
Low-grade PIN. There are mild cell changes. Most doctors do not consider this a major concern, and it does not require extra treatment.
High-grade PIN (HGPIN). There are more significant cell changes. This is watched more carefully because it is linked to a higher chance of developing prostate cancer.
If a high-grade PIN is found on a biopsy, your doctor will likely recommend more frequent follow-up and possibly repeat biopsies.
Intraductal Carcinoma of the Prostate (IDCP)
IDCP is a more advanced type of abnormal cell growth inside the prostate ducts. These are tiny tubes inside the prostate. It is more serious than PIN and is closely linked to prostate cancer.
If IDCP is found on a biopsy, you will usually need a thorough workup and close monitoring, since it is strongly associated with aggressive prostate cancer.
Proliferative Inflammatory Atrophy (PIA)
PIA is an area of the prostate where cells appear shrunken (atrophied) and show signs of past inflammation. Scientists believe PIA may be an early step in a chain of changes that can eventually lead to cancer, though most men with PIA will never develop prostate cancer.
PIA alone is not usually a cause for alarm, but it is something pathologists (doctors who study tissue samples) note and monitor.
Genetic and inherited risk factors
Some men are born with gene changes that raise their risk of developing prostate cancer. This does not mean they will definitely get cancer — it just means they may need to start screening earlier or more often.
Key genes to know about:
-
BRCA1 and BRCA2. Most people have heard of these genes in connection with breast cancer, but they also raise the risk of prostate cancer, especially BRCA2. Men with a BRCA2 mutation have a significantly higher lifetime risk and tend to develop more aggressive disease.
-
ATM, CHEK2, PALB2. These are other DNA repair genes. When they are not working correctly, the body has a harder time fixing damaged cells, which can lead to cancer.
-
HOXB13. A gene specifically linked to early-onset prostate cancer (diagnosed before age 55). Men with this mutation, especially those with a strong family history, may benefit from earlier and more frequent screening.
-
MLH1, MSH2, MSH6, PMS2 (Lynch Syndrome genes). Lynch Syndrome is a hereditary condition that increases the risk of several cancers, including prostate cancer. Men with Lynch Syndrome may also be candidates for a type of immunotherapy (a treatment that helps the immune system fight cancer).
There are also some conditions that are not linked with prostate cancer, but that affect the prostate. These share some of the early symptoms of prostate cancer, such as difficulty urinating and elevated PSA. These conditions may be mistaken for prostate cancer or make a prostate cancer diagnosis more difficult.
Benign Prostatic Hyperplasia (BPH). BPH is when the prostate is larger than it should be. "Benign" means it is NOT cancer and will NOT turn into cancer.
BPH is very common. More than half of men over 60 have it, and almost all men over 80 have some degree of it.
BPH itself is not dangerous or cancerous, but it can be uncomfortable and affect your quality of life. It can also make it harder for doctors to detect prostate cancer, since both conditions can raise your PSA (a blood test used to screen for prostate cancer).
Prostatitis. Prostatitis means the prostate is swollen or inflamed. It can be caused by a bacterial infection or by other factors that are not fully understood.
There is no proven direct link between prostatitis and prostate cancer, but chronic inflammation may play a role in prostate cancer over time. Research is still ongoing. Prostatitis can also raise PSA levels, which may cause confusion during cancer screening.
Take a look at all the prostate 101 guides
What is Prostate Cancer?
Last updated and reviewed on March 19, 2026.
Cancer begins when cells grow out of control. Prostate cancer affects the prostate gland. When you have prostate cancer, cells in the prostate do not follow the normal cell cycle. Normal cells grow, replicate (copy themselves), and then die. Cancer cells change, grow faster than normal, replicate too fast, and do not die as they should.
How does prostate cancer affect the prostate?
|
THE BASICS: When you have prostate cancer, your prostate cells grow too quickly and form a tumor. Prostate cancer is one of the most common cancers in men. It is also one of the most treatable, especially when caught early. Most men are diagnosed with prostate cancer at the localized stage. This means it has not spread to other parts of the body. Sometimes, prostate cancer can spread to other parts of the body. Around 1 in 4 men diagnosed with prostate cancer have more advanced disease at the time of diagnosis. Prostate cancer most often spreads to the bones (80%), lymph nodes (10%), liver (10%), and the lungs (9%)2. The good news is that prostate cancer often grows very slowly. Many men with early-stage prostate cancer live normal lives without needing immediate treatment. Doctors use a blood test called a PSA Test, along with imaging and biopsies, to detect and monitor it. When it does require treatment, prostate cancer treatment is often very successful, even for people with more advanced cancer.
|
What is the Prostate?

The prostate is a small gland, about the size of a walnut. It is located directly below the bladder. It surrounds the urethra, which is the tube that carries urine out of the bladder. The prostate gland produces seminal fluid. Together with sperm cells from the testicles and fluids from other glands, this fluid makes up semen.
When a person has prostate cancer, their prostate cells grow too quickly. The extra cells build up and form tumors.
How does prostate cancer affect the body?
In the early stages, prostate cancer usually does not cause pain or noticeable symptoms. The first sign of prostate cancer for many men is high levels of prostate-specific antigen (PSA) on a blood test. PSA is a protein. Small amounts of PSA are normal, but high levels of PSA can be a sign of prostate cancer or another condition affecting the prostate.
As the tumor grows, it can cause:
-
Trouble starting or stopping the flow of urine
-
A weak or interrupted urine stream
-
Needing to urinate more often, especially at night
-
A feeling that the bladder is not fully empty
-
Blood in the urine or semen
-
Pain with ejaculation
When prostate cancer spreads to other parts of the body, it most commonly affects the bones, causing pain that may wake you up at night. If it spreads to the spine, it can press on nerves and cause back pain or weakness.
Learn more about the signs and symptoms of Prostate Cancer.
Types of prostate cancer
There are several types of prostate cancer, though one type is by far the most common:
-
Acinar adenocarcinoma. The most common type of prostate cancer. It develops in the glandular cells of the prostate called acini. Acinar adenocarcinoma is what most people mean when they say "prostate cancer."
-
Ductal adenocarcinoma. A less common type that tends to grow and spread more quickly than acinar adenocarcinoma. It also begins in the gland cells of the prostate, but in the ductal cells. Sometimes prostate cancer can have both acinar and ductal cancer cells.
-
Neuroendocrine carcinoma. A rare type that starts in special cells called neuroendocrine cells. Small-cell prostate cancer is the most common form of this type and tends to grow faster than other types.
-
Adenosquamous carcinoma. A very rare type made up of two different kinds of cancer cells.
-
Sarcoma. A rare type that starts in the muscle tissue of the prostate.
-
Lymphoma. A very rare type where cancer of the lymph system starts in the prostate. Most of the time, prostate lymphoma is a type of non-Hodgkin lymphoma.
Prostate cancer subtypes
Within those main types, doctors can break prostate cancer down even further into subtypes. There are two ways to look at subtypes:
By How the Cells Look (Histological Subtypes)
When a doctor looks at prostate cancer cells under a microscope, they can sometimes see special patterns that help identify a subtype. Some examples include:
-
Signet-cell-like adenocarcinoma. Cancer cells that look like signet rings under a microscope.
-
Sarcomatoid carcinoma. A rare and aggressive form where cancer cells look like sarcoma cells.
-
Squamous cell carcinoma. A very rare form that develops from flat cells lining the prostate.
-
Adenoid cystic carcinoma. A very rare, slow-growing subtype that begins in the basal cells of the prostate.
Recognizing these subtypes is important. It can help identify prostate cancer that grows more quickly and help choose treatments.
By the Genes Inside the Cancer Cells (Molecular Subtypes)
Scientists have also found that prostate cancer can be broken down into subtypes based on changes in the genes inside the cancer cells. Think of genes like instructions inside a cell. When those instructions get changed or damaged, cancer can develop.
Some of the most common gene changes found in prostate cancer include:
-
ERG gene fusions. The most common gene change is found in about half of all prostate cancers.
-
SPOP mutations. Found in about 1 in 10 prostate cancers.
-
FOXA1 mutations. A less common gene change.
Understanding the gene changes in a person's prostate cancer is becoming increasingly important. This is because it helps doctors choose the best treatment and predict how the cancer may behave over time.
What are the related disorders to prostate cancer?
The following conditions are not cancer, but they are changes in the prostate cells that doctors watch carefully because they can sometimes lead to cancer. These are sometimes known as precursor conditions or precancerous conditions.
Prostatic Intraepithelial Neoplasia (PIN)
PIN means some of the cells lining the prostate look abnormal under a microscope. Think of it as cells that have started to look "different" but have not yet grown into surrounding tissue. There are two types:
-
Low-grade PIN. There are mild cell changes. Most doctors do not consider this a major concern, and it does not require extra treatment.
-
High-grade PIN (HGPIN). There are more significant cell changes. This is watched more carefully because it is linked to a higher chance of developing prostate cancer.
If a high-grade PIN is found on a biopsy, your doctor will likely recommend more frequent follow-up and possibly repeat biopsies.
Intraductal Carcinoma of the Prostate (IDCP)
IDCP is a more advanced type of abnormal cell growth inside the prostate ducts. These are tiny tubes inside the prostate. It is more serious than PIN and is closely linked to prostate cancer.
If IDCP is found on a biopsy, you will usually need a thorough workup and close monitoring, since it is strongly associated with aggressive prostate cancer.
Proliferative Inflammatory Atrophy (PIA)
PIA is an area of the prostate where cells appear shrunken (atrophied) and show signs of past inflammation. Scientists believe PIA may be an early step in a chain of changes that can eventually lead to cancer, though most men with PIA will never develop prostate cancer.
PIA alone is not usually a cause for alarm, but it is something pathologists (doctors who study tissue samples) note and monitor.
Genetic and inherited risk factors
Some men are born with gene changes that raise their risk of developing prostate cancer. This does not mean they will definitely get cancer — it just means they may need to start screening earlier or more often.
Key genes to know about:
-
BRCA1 and BRCA2. Most people have heard of these genes in connection with breast cancer, but they also raise the risk of prostate cancer, especially BRCA2. Men with a BRCA2 mutation have a significantly higher lifetime risk and tend to develop more aggressive disease.
-
ATM, CHEK2, PALB2. These are other DNA repair genes. When they are not working correctly, the body has a harder time fixing damaged cells, which can lead to cancer.
-
HOXB13. A gene specifically linked to early-onset prostate cancer (diagnosed before age 55). Men with this mutation, especially those with a strong family history, may benefit from earlier and more frequent screening.
-
MLH1, MSH2, MSH6, PMS2 (Lynch Syndrome genes). Lynch Syndrome is a hereditary condition that increases the risk of several cancers, including prostate cancer. Men with Lynch Syndrome may also be candidates for a type of immunotherapy (a treatment that helps the immune system fight cancer).
There are also some conditions that are not linked with prostate cancer, but that affect the prostate. These share some of the early symptoms of prostate cancer, such as difficulty urinating and elevated PSA. These conditions may be mistaken for prostate cancer or make a prostate cancer diagnosis more difficult.
Benign Prostatic Hyperplasia (BPH). BPH is when the prostate is larger than it should be. "Benign" means it is NOT cancer and will NOT turn into cancer.
BPH is very common. More than half of men over 60 have it, and almost all men over 80 have some degree of it.
BPH itself is not dangerous or cancerous, but it can be uncomfortable and affect your quality of life. It can also make it harder for doctors to detect prostate cancer, since both conditions can raise your PSA (a blood test used to screen for prostate cancer).
Prostatitis. Prostatitis means the prostate is swollen or inflamed. It can be caused by a bacterial infection or by other factors that are not fully understood.
There is no proven direct link between prostatitis and prostate cancer, but chronic inflammation may play a role in prostate cancer over time. Research is still ongoing. Prostatitis can also raise PSA levels, which may cause confusion during cancer screening.
Take a look at all the prostate 101 guides
Trending Articles
Get the Latest Prostate Cancer Updates, Delivered to You.
By subscribing to the HealthTree newsletter, you'll receive the latest research, treatment updates, and expert insights to help you navigate your health.
Together we care.
Together we cure.