Understanding Treating Prostate Cancer
How is Prostate Cancer Treated?
Last updated and reviewed on March 26, 2026.
The treatment for prostate cancer depends on various factors, such as the stage of the cancer, the patient’s age and overall health, and whether the prostate cancer is newly diagnosed or has come back.
Treatment often involves a combination of these therapies tailored to the individual patient’s needs. It's important for patients to discuss all treatment options with their healthcare team to make the best decision for their unique situation.
After your diagnosis, it is normal to get a second opinion. During a second opinion, another oncologist will look at your biopsy results and other tests you had during your diagnosis. They will offer their opinion on your treatment.
Active surveillance for prostate cancer
What is active surveillance for prostate cancer?
During active surveillance, your doctor monitors your prostate cancer over time. It is also called “watch and wait” or “watchful waiting.” You will have regular blood tests, check-ups, and occasional biopsies to make sure the cancer is not growing.
Who is active surveillance for?
Men with slow-growing, low-risk prostate cancer that is unlikely to cause problems anytime soon. Active surveillance is not a good option for people with higher-risk prostate cancer.
What is the benefit of active surveillance?
Active surveillance avoids the side effects of treatment for as long as possible, sometimes indefinitely. Many men on active surveillance never need treatment at all.
What should I know about active surveillance?
It is important to know that active surveillance is not "doing nothing." It is a deliberate, carefully managed plan. If the cancer starts to grow, treatment will begin. Research has shown that for men with low-risk prostate cancer, active surveillance is an effective way to manage the cancer.
Surgery (radical prostatectomy) for prostate cancer
What is a radical prostatectomy?
The main surgery for prostate cancer is called a radical prostatectomy. A surgeon, called a urologist, removes the entire prostate gland. Some tissue around the prostate gland is also removed. Lymph nodes near the prostate cancer may also be removed.
Today, most surgeries are done using a robotic-assisted system, which allows for smaller cuts, less blood loss, and a faster recovery.
Who is a radical prostatectomy for?
Men with cancer that is still contained within the prostate and who are healthy enough for surgery.
What should I know?
Possible side effects include urinary leakage (incontinence) and sexual dysfunction (erectile dysfunction). These effects often improve over time, but may be permanent for some men. A radical prostatectomy also causes infertility. This is the inability to conceive a child. If it is important to you, talk to your doctor about your options before surgery.
Other possible side effects include:
-
Bleeding
-
Blood clots
-
Infection
Radiation therapy for prostate cancer
What is it?
Radiation uses high-energy beams to kill cancer cells. There are two main types:
-
External beam radiation therapy (EBRT): A machine outside your body aims targeted radiation at the prostate. Modern techniques like intensity-modulated radiation therapy (IMRT) and stereotactic body radiation therapy (SBRT) are very precise. This reduces damage to surrounding healthy tissue. Treatment is typically given over several weeks.
-
Brachytherapy or internal radiation therapy: Tiny radioactive seeds are placed directly inside the prostate through a needle. The seeds release radiation slowly over time to kill the cancer from the inside.
Who is it for?
Radiation therapy is used for both early-stage and more advanced prostate cancer. Radiation therapy is used:
-
For lower-risk prostate cancer that is still in the prostate gland
For higher-risk prostate cancer that is still in the prostate or has grown into nearby tissue, in combination with hormone therapy
After surgery if the surgery does not remove all cancer cells
After cancer recurrence after surgery to remove the prostate
For advanced prostate cancer, to help control the cancer and relieve symptoms
What should I know?
Side effects can include urinary, bowel, and sexual problems, though modern techniques minimize these risks. Other side effects include fatigue and lymphedema, which is swelling, in the legs or genital area.
Hormone therapy for prostate cancer
What is it?
Hormone therapy for prostate cancer is also known as androgen deprivation therapy (ADT). Prostate cancer needs the male hormone testosterone to grow. Hormone therapy lowers testosterone levels in your body to slow or stop cancer growth. This can be done with medications (injections or pills) or, less commonly, with surgery to remove the testicles. This surgery is called an orchiectomy or surgical castration.
Common hormone therapy medications include:
- Abiraterone (Zytiga)
- Apalutamide (Erleada)
- Enzalutamide (Xtandi)
- Leuprolide (Lupron, Eligard)
Who is it for?
Hormone therapy is used for men with cancer that has spread beyond the prostate. It can be used in addition to radiation therapy, surgery, and other treatments.
What should I know?
Side effects can include hot flashes, fatigue, loss of sex drive, weight gain, and bone thinning. Your doctor can help manage these effects.
Chemotherapy for prostate cancer
What is it?
Chemotherapy uses powerful drugs to kill fast-growing cancer cells throughout the body. It is given through an IV (into a vein) in cycles, with rest periods in between. Some chemotherapies are given as a pill.
The most common first chemotherapy regimen for prostate cancer is docetaxel. Other examples of chemotherapy for prostate cancer include:
- Cabazitaxel (Jevtana)
- Carboplatin (Paraplatin)
- Estramustine (Emcyt)
- Mitoxantrone (Novantrone)
Who is it for?
Chemotherapy is used for advanced prostate cancer that has spread to other parts of the body. It is also used for prostate cancer that is no longer responding to hormone therapy.
What should I know?
Chemotherapy can cause side effects like nausea, fatigue, mouth sores, appetite loss, hair loss, neuropathy, and a higher risk of infection. Your care team will monitor you closely throughout treatment.
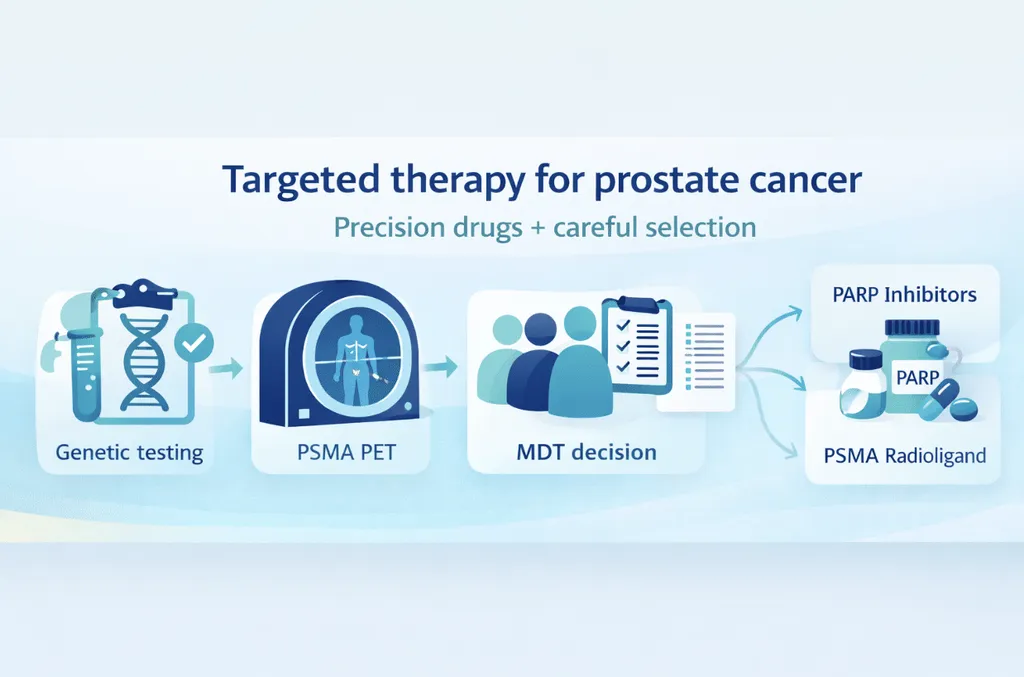
Targeted therapy for prostate cancer
What is it?
Some men have changes (mutations) in their DNA that help cancer cells survive. These include mutations to the BRCA1 or BRCA2 genes. Targeted therapy is a type of cancer treatment that targets specific molecules on cancer cells. PARP inhibitors are drugs that block a pathway cancer cells use to repair themselves, causing them to die. PARP inhibitors that are approved to treat prostate cancer include:
- Niraparib plus abiraterone (Akeega)
- Olaparib (Lynparza)
- Rucaparib (Rubraca)
- Talazoparib (Talzenna)
PARP inhibitors may be given with hormone therapy, with chemotherapy, or by themselves.
Who is it for?
Men with advanced prostate cancer who have specific gene mutations. Your doctor may recommend genetic testing to find out if this applies to you.
What should I know?
This is a newer and more precise approach that targets cancer cells specifically, which can mean fewer side effects than traditional chemotherapy. PARP inhibitors can cause nausea, vomiting, diarrhea, fatigue, appetite loss, low red blood cell counts (anemia), and other side effects.
Immunotherapy for prostate cancer
What is it?
Immunotherapy is a type of cancer treatment that helps your own immune system recognize and fight cancer cells. Sipuleucel-T (Provenge) is a cancer vaccine. It is a unique treatment where doctors take immune cells from your own blood, train them in a lab to fight prostate cancer, and then put them back into your body through an IV. It is usually given before chemotherapy.
Sometimes, a type of immunotherapy called an immune checkpoint inhibitor may be used for prostate cancer. Pembrolizumab (Keytruda) can be used for advanced prostate cancer that has progressed after treatment, has certain features found on a lab test, and has no other treatment options. These are microsatellite instability-high (MSI-H0, mismatch repair deficiency (dMMR), and/or high tumor mutational burden (TMB-H).
Who is it for?
Men with advanced prostate cancer that is no longer responding to hormone therapy.
What should I know?
It does not shrink tumors, but it has been shown to help some men live longer. Side effects are generally mild flu-like symptoms after infusions.
Radioligand therapy (Lutetium-177 PSMA) for prostate cancer
What is it?
This is a newer, highly targeted treatment. It is a radiopharmaceutical, which is a radioactive medication. A radioactive substance is attached to a molecule that seeks out prostate cancer cells by targeting a protein on their surface called PSMA. Once it finds the cancer cells, it delivers radiation directly to them. This minimizes damage to healthy tissue. It is called lutetium-177 PSMA-617 (Pluvicto)
Who is it for?
Men with advanced prostate cancer that has spread and is no longer responding to hormone therapy or chemotherapy.
What should I know?
This is one of the most exciting recent advances in prostate cancer treatment. Your doctor will test whether your cancer expresses PSMA using a special scan before recommending this option.
Cryotherapy for prostate cancer
What is it?
Cryotherapy is a type of ablative treatment. This type of treatment is minimally invasive and uses cold temperatures to freeze and destroy cancer cells. A probe is inserted near the prostate to deliver the cold temperature to the cancer cells.
Who is it for?
Some men with early-stage, localized prostate cancer, or as a second treatment if radiation has not fully worked.
What should I know?
This is a less commonly used treatment option. For some men with low-risk, early-stage prostate cancer, it may be a treatment option if they can’t have radiation therapy or surgery.
Supportive care during treatment
Treating the symptoms of cancer and side effects of cancer treatment is called palliative and supportive care. This is an important part of your cancer treatment.
There is a common misconception that palliative care is only given at the end of life. Palliative and supportive care can be given at any time during cancer treatment.
It is important to talk to your care team about the symptoms and side effects you are feeling. Tell them how much they are affecting your day-to-day life. They may be able to adjust your treatment schedule, change medications, or treat the symptom or side effect directly to help you feel better.
Palliative and supportive care can include pain management, physical therapy, nutritional support, and psychological support.
Follow-up care after treatment ends
After active cancer treatment ends, your care continues. Your health care team will help make a follow-up plan that you should follow closely. It will help check if the cancer comes back and manage long-term side effects.
For prostate cancer, it is important to continue to watch for a cancer recurrence. This is when the cancer comes back after treatment ends. After treatment ends, you will need PSA tests every 6 months for the first 5 years and then once a year. If you are getting ongoing treatment, you may need tests more frequently. You may also need regular imaging tests.
Men with prostate cancer are also at a higher risk of secondary cancers. A secondary cancer is when you get a different cancer from your original diagnosis. Prostate cancer survivors are at a higher risk of:
- Acute myeloid leukemia (AML)
- Bladder cancer
- Melanoma
- Small intestine cancer
- Soft tissue sarcoma
- Thymus cancer
- Thyroid cancer
How is Prostate Cancer Treated?
Last updated and reviewed on March 26, 2026.
The treatment for prostate cancer depends on various factors, such as the stage of the cancer, the patient’s age and overall health, and whether the prostate cancer is newly diagnosed or has come back.
Treatment often involves a combination of these therapies tailored to the individual patient’s needs. It's important for patients to discuss all treatment options with their healthcare team to make the best decision for their unique situation.
After your diagnosis, it is normal to get a second opinion. During a second opinion, another oncologist will look at your biopsy results and other tests you had during your diagnosis. They will offer their opinion on your treatment.
Active surveillance for prostate cancer
What is active surveillance for prostate cancer?
During active surveillance, your doctor monitors your prostate cancer over time. It is also called “watch and wait” or “watchful waiting.” You will have regular blood tests, check-ups, and occasional biopsies to make sure the cancer is not growing.
Who is active surveillance for?
Men with slow-growing, low-risk prostate cancer that is unlikely to cause problems anytime soon. Active surveillance is not a good option for people with higher-risk prostate cancer.
What is the benefit of active surveillance?
Active surveillance avoids the side effects of treatment for as long as possible, sometimes indefinitely. Many men on active surveillance never need treatment at all.
What should I know about active surveillance?
It is important to know that active surveillance is not "doing nothing." It is a deliberate, carefully managed plan. If the cancer starts to grow, treatment will begin. Research has shown that for men with low-risk prostate cancer, active surveillance is an effective way to manage the cancer.
Surgery (radical prostatectomy) for prostate cancer
What is a radical prostatectomy?
The main surgery for prostate cancer is called a radical prostatectomy. A surgeon, called a urologist, removes the entire prostate gland. Some tissue around the prostate gland is also removed. Lymph nodes near the prostate cancer may also be removed.
Today, most surgeries are done using a robotic-assisted system, which allows for smaller cuts, less blood loss, and a faster recovery.
Who is a radical prostatectomy for?
Men with cancer that is still contained within the prostate and who are healthy enough for surgery.
What should I know?
Possible side effects include urinary leakage (incontinence) and sexual dysfunction (erectile dysfunction). These effects often improve over time, but may be permanent for some men. A radical prostatectomy also causes infertility. This is the inability to conceive a child. If it is important to you, talk to your doctor about your options before surgery.
Other possible side effects include:
-
Bleeding
-
Blood clots
-
Infection
Radiation therapy for prostate cancer
What is it?
Radiation uses high-energy beams to kill cancer cells. There are two main types:
-
External beam radiation therapy (EBRT): A machine outside your body aims targeted radiation at the prostate. Modern techniques like intensity-modulated radiation therapy (IMRT) and stereotactic body radiation therapy (SBRT) are very precise. This reduces damage to surrounding healthy tissue. Treatment is typically given over several weeks.
-
Brachytherapy or internal radiation therapy: Tiny radioactive seeds are placed directly inside the prostate through a needle. The seeds release radiation slowly over time to kill the cancer from the inside.
Who is it for?
Radiation therapy is used for both early-stage and more advanced prostate cancer. Radiation therapy is used:
-
For lower-risk prostate cancer that is still in the prostate gland
-
For higher-risk prostate cancer that is still in the prostate or has grown into nearby tissue, in combination with hormone therapy
-
After surgery if the surgery does not remove all cancer cells
-
After cancer recurrence after surgery to remove the prostate
-
For advanced prostate cancer, to help control the cancer and relieve symptoms
What should I know?
Side effects can include urinary, bowel, and sexual problems, though modern techniques minimize these risks. Other side effects include fatigue and lymphedema, which is swelling, in the legs or genital area.
Hormone therapy for prostate cancer
What is it?
Hormone therapy for prostate cancer is also known as androgen deprivation therapy (ADT). Prostate cancer needs the male hormone testosterone to grow. Hormone therapy lowers testosterone levels in your body to slow or stop cancer growth. This can be done with medications (injections or pills) or, less commonly, with surgery to remove the testicles. This surgery is called an orchiectomy or surgical castration.
Common hormone therapy medications include:
- Abiraterone (Zytiga)
- Apalutamide (Erleada)
- Enzalutamide (Xtandi)
- Leuprolide (Lupron, Eligard)
Who is it for?
Hormone therapy is used for men with cancer that has spread beyond the prostate. It can be used in addition to radiation therapy, surgery, and other treatments.
What should I know?
Side effects can include hot flashes, fatigue, loss of sex drive, weight gain, and bone thinning. Your doctor can help manage these effects.
Chemotherapy for prostate cancer
What is it?
Chemotherapy uses powerful drugs to kill fast-growing cancer cells throughout the body. It is given through an IV (into a vein) in cycles, with rest periods in between. Some chemotherapies are given as a pill.
The most common first chemotherapy regimen for prostate cancer is docetaxel. Other examples of chemotherapy for prostate cancer include:
- Cabazitaxel (Jevtana)
- Carboplatin (Paraplatin)
- Estramustine (Emcyt)
- Mitoxantrone (Novantrone)
Who is it for?
Chemotherapy is used for advanced prostate cancer that has spread to other parts of the body. It is also used for prostate cancer that is no longer responding to hormone therapy.
What should I know?
Chemotherapy can cause side effects like nausea, fatigue, mouth sores, appetite loss, hair loss, neuropathy, and a higher risk of infection. Your care team will monitor you closely throughout treatment.
Targeted therapy for prostate cancer
What is it?
Some men have changes (mutations) in their DNA that help cancer cells survive. These include mutations to the BRCA1 or BRCA2 genes. Targeted therapy is a type of cancer treatment that targets specific molecules on cancer cells. PARP inhibitors are drugs that block a pathway cancer cells use to repair themselves, causing them to die. PARP inhibitors that are approved to treat prostate cancer include:
- Niraparib plus abiraterone (Akeega)
- Olaparib (Lynparza)
- Rucaparib (Rubraca)
- Talazoparib (Talzenna)
PARP inhibitors may be given with hormone therapy, with chemotherapy, or by themselves.
Who is it for?
Men with advanced prostate cancer who have specific gene mutations. Your doctor may recommend genetic testing to find out if this applies to you.
What should I know?
This is a newer and more precise approach that targets cancer cells specifically, which can mean fewer side effects than traditional chemotherapy. PARP inhibitors can cause nausea, vomiting, diarrhea, fatigue, appetite loss, low red blood cell counts (anemia), and other side effects.
Immunotherapy for prostate cancer
What is it?
Immunotherapy is a type of cancer treatment that helps your own immune system recognize and fight cancer cells. Sipuleucel-T (Provenge) is a cancer vaccine. It is a unique treatment where doctors take immune cells from your own blood, train them in a lab to fight prostate cancer, and then put them back into your body through an IV. It is usually given before chemotherapy.
Sometimes, a type of immunotherapy called an immune checkpoint inhibitor may be used for prostate cancer. Pembrolizumab (Keytruda) can be used for advanced prostate cancer that has progressed after treatment, has certain features found on a lab test, and has no other treatment options. These are microsatellite instability-high (MSI-H0, mismatch repair deficiency (dMMR), and/or high tumor mutational burden (TMB-H).
Who is it for?
Men with advanced prostate cancer that is no longer responding to hormone therapy.
What should I know?
It does not shrink tumors, but it has been shown to help some men live longer. Side effects are generally mild flu-like symptoms after infusions.
Radioligand therapy (Lutetium-177 PSMA) for prostate cancer
What is it?
This is a newer, highly targeted treatment. It is a radiopharmaceutical, which is a radioactive medication. A radioactive substance is attached to a molecule that seeks out prostate cancer cells by targeting a protein on their surface called PSMA. Once it finds the cancer cells, it delivers radiation directly to them. This minimizes damage to healthy tissue. It is called lutetium-177 PSMA-617 (Pluvicto)
Who is it for?
Men with advanced prostate cancer that has spread and is no longer responding to hormone therapy or chemotherapy.
What should I know?
This is one of the most exciting recent advances in prostate cancer treatment. Your doctor will test whether your cancer expresses PSMA using a special scan before recommending this option.
Cryotherapy for prostate cancer
What is it?
Cryotherapy is a type of ablative treatment. This type of treatment is minimally invasive and uses cold temperatures to freeze and destroy cancer cells. A probe is inserted near the prostate to deliver the cold temperature to the cancer cells.
Who is it for?
Some men with early-stage, localized prostate cancer, or as a second treatment if radiation has not fully worked.
What should I know?
This is a less commonly used treatment option. For some men with low-risk, early-stage prostate cancer, it may be a treatment option if they can’t have radiation therapy or surgery.
Supportive care during treatment
Treating the symptoms of cancer and side effects of cancer treatment is called palliative and supportive care. This is an important part of your cancer treatment.
There is a common misconception that palliative care is only given at the end of life. Palliative and supportive care can be given at any time during cancer treatment.
It is important to talk to your care team about the symptoms and side effects you are feeling. Tell them how much they are affecting your day-to-day life. They may be able to adjust your treatment schedule, change medications, or treat the symptom or side effect directly to help you feel better.
Palliative and supportive care can include pain management, physical therapy, nutritional support, and psychological support.
Follow-up care after treatment ends
After active cancer treatment ends, your care continues. Your health care team will help make a follow-up plan that you should follow closely. It will help check if the cancer comes back and manage long-term side effects.
For prostate cancer, it is important to continue to watch for a cancer recurrence. This is when the cancer comes back after treatment ends. After treatment ends, you will need PSA tests every 6 months for the first 5 years and then once a year. If you are getting ongoing treatment, you may need tests more frequently. You may also need regular imaging tests.
Men with prostate cancer are also at a higher risk of secondary cancers. A secondary cancer is when you get a different cancer from your original diagnosis. Prostate cancer survivors are at a higher risk of:
- Acute myeloid leukemia (AML)
- Bladder cancer
- Melanoma
- Small intestine cancer
- Soft tissue sarcoma
- Thymus cancer
- Thyroid cancer
Get the Latest Prostate Cancer Updates, Delivered to You.
By subscribing to the HealthTree newsletter, you'll receive the latest research, treatment updates, and expert insights to help you navigate your health.
Together we care.
Together we cure.